Introduction
Imagine waking up to a world that’s slowly fading away—colors dimming, faces blurring, and details slipping out of reach. For millions of people with diabetes, this isn’t just a scary thought; it’s a reality called Diabetic Retinopathy.
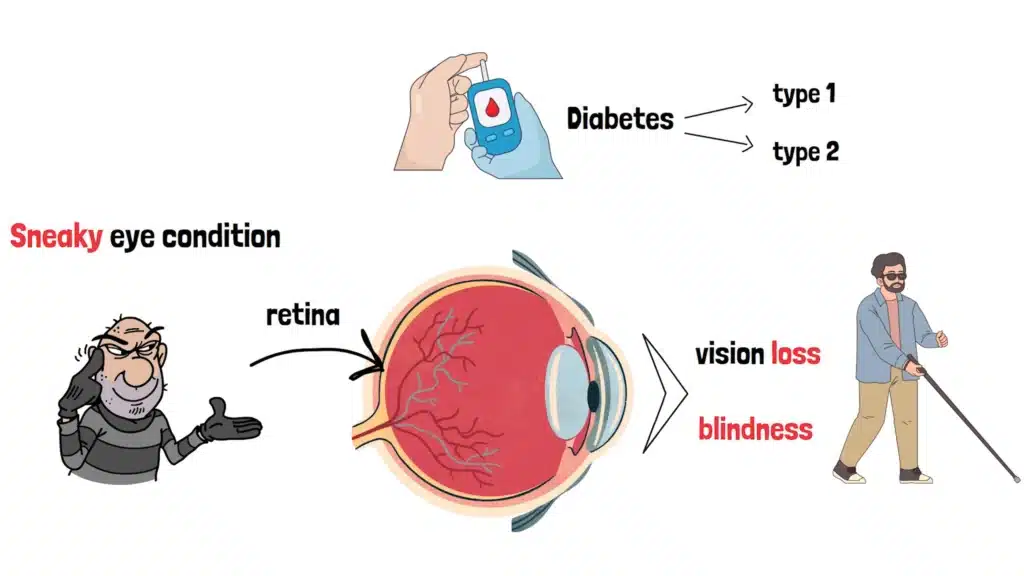
So, what is it? Diabetic Retinopathy is a sneaky eye condition that damages the retina, the light-sensitive layer at the back of your eye. It’s a complication of diabetes, and it can affect anyone with type 1 or type 2 diabetes, especially if their blood sugar levels are poorly controlled. Left unchecked, it can lead to vision loss or even blindness.
But here’s the good news: with the right knowledge and care, you can protect your sight. That’s why we’re here today—to arm you with everything you need to know about Diabetic Retinopathy, from what causes it to how to prevent it. So, let’s dive in and shed some light on this condition.
What Causes Diabetic Retinopathy?
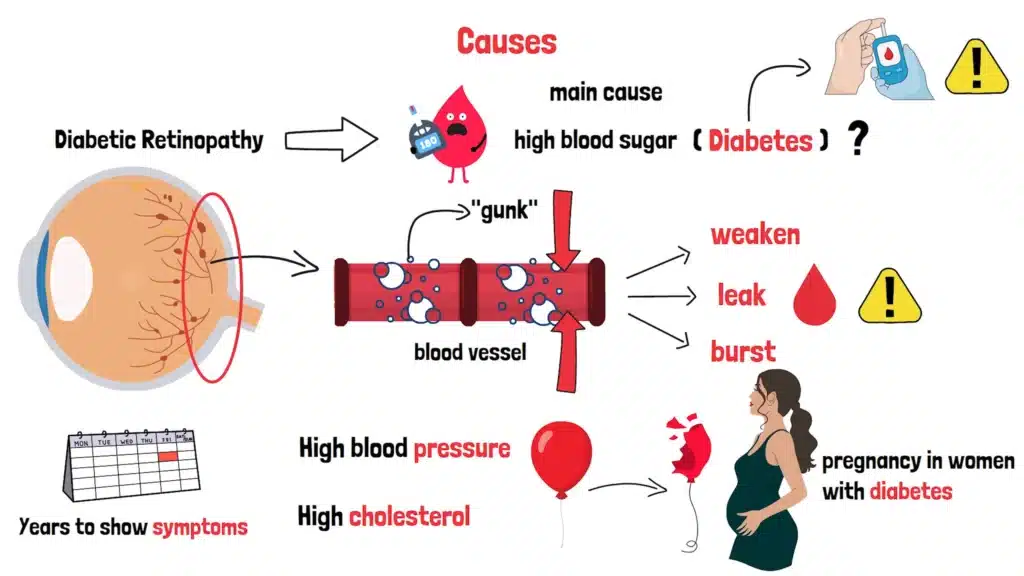
At the heart of Diabetic Retinopathy is one main culprit: high blood sugar. But how does it wreak havoc on your eyes? Let’s break it down.
Think of the blood vessels in your retina as tiny, delicate pipes. When your blood sugar levels are too high for too long, it’s like gunk building up inside those pipes. Over time, this “gunk” causes the vessels to weaken, leak, or even burst. That leakage can damage the retina, leading to vision problems. It’s a slow process, often taking years to show symptoms, which is why it’s so sneaky.
But diabetes isn’t the only player here. High blood pressure and high cholesterol can make things worse, like adding extra pressure to those already fragile pipes. Imagine trying to hold a water balloon that’s about to burst—any extra squeeze can cause a disaster. That’s what these additional conditions do to your retinal vessels.
Here’s something you might not know: the longer you’ve had diabetes, the higher your risk. Other factors, like pregnancy in women with diabetes, can also speed up the process. So, while high blood sugar is the main cause, it’s not working alone. Understanding these causes is the first step to protecting your vision.
Risk Factors for Diabetic Retinopathy
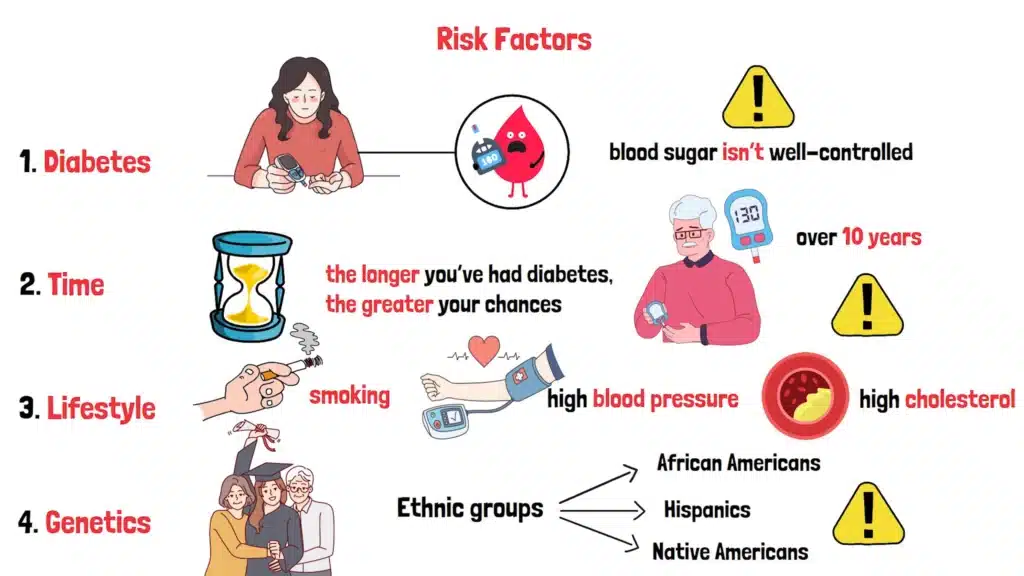
Who’s most at risk for Diabetic Retinopathy? If you have diabetes, you’re already on the list—especially if your blood sugar isn’t well-controlled. But there are other factors that can push your risk even higher.
Duration of Diabetes
The longer you’ve had diabetes, the greater your chances. For example, if you’ve had diabetes for over 10 years, your risk climbs significantly. Age plays a role too, as older adults are more susceptible.
Lifestyle and Health Factors
Then there are lifestyle factors. Smoking? It’s like adding fuel to the fire, damaging your blood vessels even more. High blood pressure and high cholesterol also increase your risk, as they put extra strain on your retinal vessels. If your parents had Diabetic Retinopathy, your odds might climb too, thanks to genetics.
Genetic and Ethnic Considerations
Here’s a surprising one: certain ethnic groups, like African Americans, Hispanics, and Native Americans, face a higher risk.
But don’t worry—some of these factors, like smoking and blood pressure, are things you can control. By understanding what makes you vulnerable, you can take steps to protect yourself.
Symptoms of Diabetic Retinopathy: What to Watch For
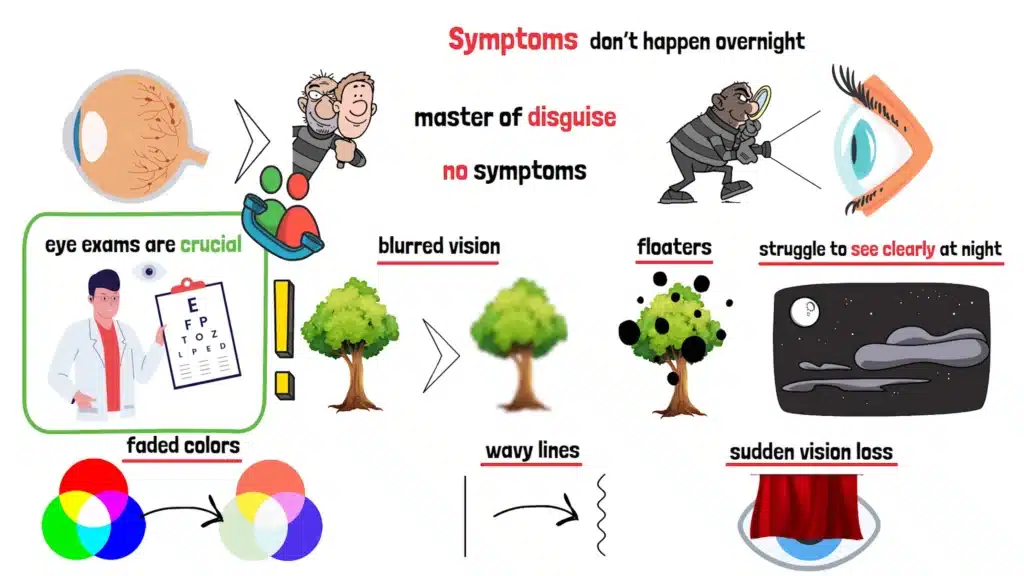
Diabetic Retinopathy is a master of disguise. In its early stages, it often has no symptoms at all—like a thief sneaking in without making a sound. That’s why regular eye exams are so crucial. But as the condition progresses, you might start to notice changes.
Early Warning Signs
- Blurred vision – like trying to see through a foggy window
- Dark spots or “floaters” – drifting across your field of view, as if someone sprinkled pepper in the air
- Difficulty seeing at night – like the world is dimming around you
- Faded colors – the world losing its vibrancy
- Wavy lines – straight lines appearing distorted
Advanced Symptoms
As it worsens, you might struggle to see clearly at night, like the world is dimming around you. Colors might fade, and straight lines could appear wavy. In the most advanced stages, you could experience sudden vision loss—like a curtain falling over your eyes. It’s alarming, but remember: these symptoms don’t happen overnight. They creep in slowly, which is why paying attention to even small changes is key.
If you notice any of these signs, don’t panic—but don’t ignore them either. Schedule an eye exam. Early detection can make all the difference. Your vision is precious, and being aware of these symptoms is your first line of defense.
How Diabetic Retinopathy Is Diagnosed
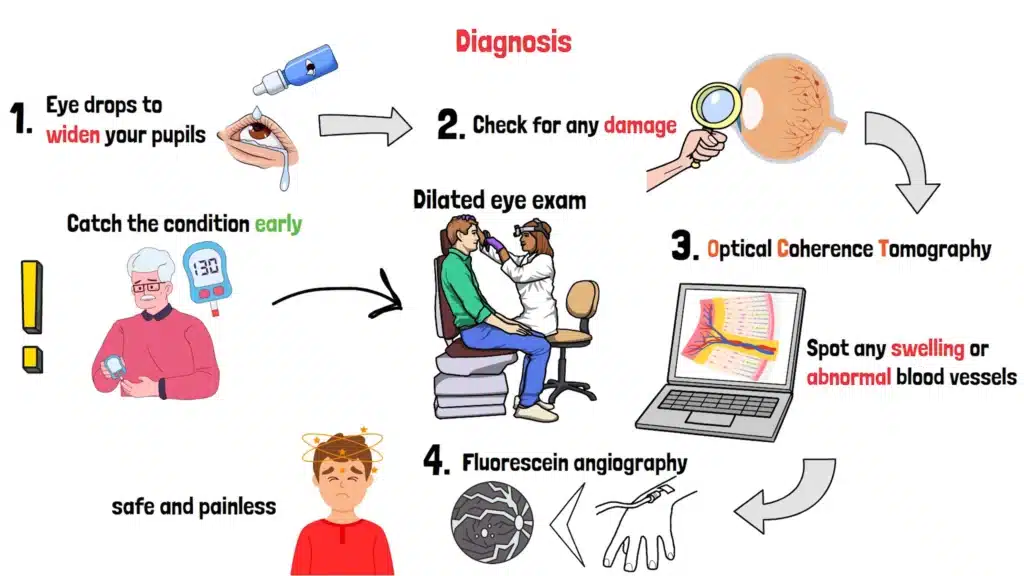
So, how do doctors diagnose Diabetic Retinopathy? It all starts with a comprehensive dilated eye exam. First, the doctor will put drops in your eyes to widen your pupils. It might sting a little, but it’s quick. Then, using a special lens, they’ll take a close look at your retina to check for any damage.
Advanced Diagnostic Techniques
If they need more detail, they might use:
- Optical Coherence Tomography (OCT) – This test creates a detailed image of your retina, almost like a 3D map, to spot any swelling or abnormal blood vessels
- Fluorescein Angiography – This involves injecting a dye into your arm and taking pictures as it flows through your retinal vessels. It helps the doctor see if any vessels are leaking or blocked
These advanced imaging techniques provide your eye care professional with the detailed information needed to develop an effective treatment plan.
Treatment Options for Diabetic Retinopathy
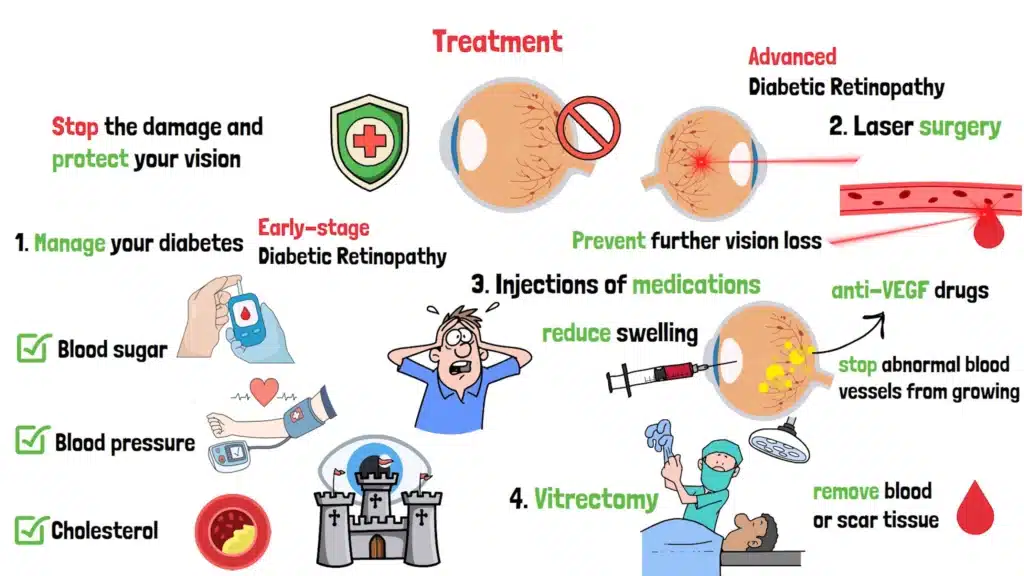
When it comes to treating Diabetic Retinopathy, the goal is simple: stop the damage and protect your vision. But the approach depends on how advanced the condition is. Let’s start with the foundation—managing your diabetes. Keeping your blood sugar, blood pressure, and cholesterol in check is like building a strong fortress around your eyes. It won’t reverse the damage, but it can slow or even stop the progression.
For early-stage Diabetic Retinopathy, that might be all you need. But if the condition is more advanced, there are other options. Laser surgery is a common treatment. It’s not as scary as it sounds—the laser seals leaking blood vessels or shrinks abnormal ones. Think of it like cauterizing a wound to stop the bleeding. It can help prevent further vision loss, but it might not bring back what’s already gone.
Another option is injections of medications, like anti-VEGF drugs, directly into the eye. These help reduce swelling and stop abnormal blood vessels from growing. Yes, the idea of an eye injection might make you squirm, but it’s quick, and numbing drops make it manageable. Plus, it can be highly effective.
In severe cases, you might need a vitrectomy—a surgery to remove blood or scar tissue from the eye. It’s more invasive, but it can restore some vision if done in time.
Prevention and Management Strategies

Preventing Diabetic Retinopathy starts with one golden rule: manage your diabetes. Monitor your blood sugar levels regularly, take your medications as prescribed, and follow a healthy diet. Exercise is your friend too. And if you smoke, quitting is one of the best things you can do for your eyes, and your overall health.
But prevention isn’t just about diabetes. Protect your eyes from UV light by wearing sunglasses, and keep your blood pressure and cholesterol in check.
Even if you already have Diabetic Retinopathy, these steps can help manage it and slow its progression. And here’s something you can do today: schedule regular eye exams. If you haven’t had one in the past year, pick up the phone and make an appointment. It’s a small step that can make a big difference.
Living with Diabetic Retinopathy: Impact on Daily Life
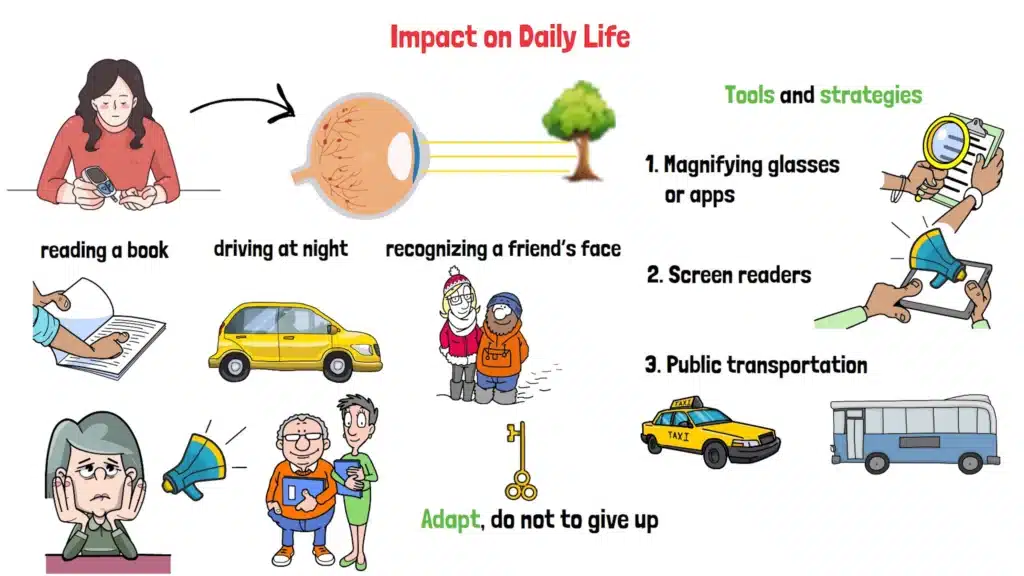
Living with Diabetic Retinopathy can feel like navigating a world that’s slowly losing its sharpness. Simple tasks—like reading a book, driving at night, or even recognizing a friend’s face—can become challenging.
But here’s the thing: you don’t have to face it alone. There are tools and strategies to help. Magnifying glasses or apps can make reading easier. Screen readers can turn text into speech on your devices. And if driving becomes tricky, public transportation or ride-sharing services can keep you mobile.
Socially, it might feel isolating if you can’t see faces clearly, but open communication helps. Let your friends and family know what you’re going through—they’ll likely be eager to support you.
The key is to adapt, not to give up. Many people with Diabetic Retinopathy lead full, active lives by making small adjustments.
Current Research and Future Developments
The future looks promising for Diabetic Retinopathy treatment. Scientists are exploring exciting new avenues, like gene therapy, which could one day repair damaged retinal cells. Another area of research is stem cell therapy, where stem cells might be used to regenerate healthy retinal tissue.
There’s also progress in medications. Newer anti-VEGF drugs are being tested to see if they can be more effective or require fewer injections. And for those who can’t undergo current treatments, researchers are working on oral medications that could offer a less invasive option.
In the meantime, the best way to protect your vision is through early detection and proper diabetes management.
Conclusion
Diabetic Retinopathy might be a serious condition, but it’s not unbeatable. Let’s recap: it’s caused by high blood sugar damaging the retina, and it can sneak up without symptoms. Regular eye exams are your best defense. Managing your diabetes—through diet, exercise, and medication—is crucial. If you notice any changes in your vision, don’t wait—talk to an eye doctor. With early detection and treatment, many people preserve their sight and continue living full lives.
If you have diabetes, schedule an eye exam today. And if you’re overdue for one, make that appointment now. Your vision is irreplaceable, but with the right care, you can protect it. Remember, you’re in control. Stay informed, stay proactive, and keep looking forward—because a clear future is worth every effort.



