Hypertensive retinopathy is damage to the light-sensitive tissue at the back of your eye caused by high blood pressure. This tissue is called the retina and it’s absolutely crucial for your vision. When you have sustained high blood pressure over a long period of time, the blood vessels in your retina become damaged and weakened. Think of your retina as the sensitive film inside a camera that captures images. When high blood pressure damages these delicate blood vessels, the retina cannot receive the proper blood supply it needs to function correctly.
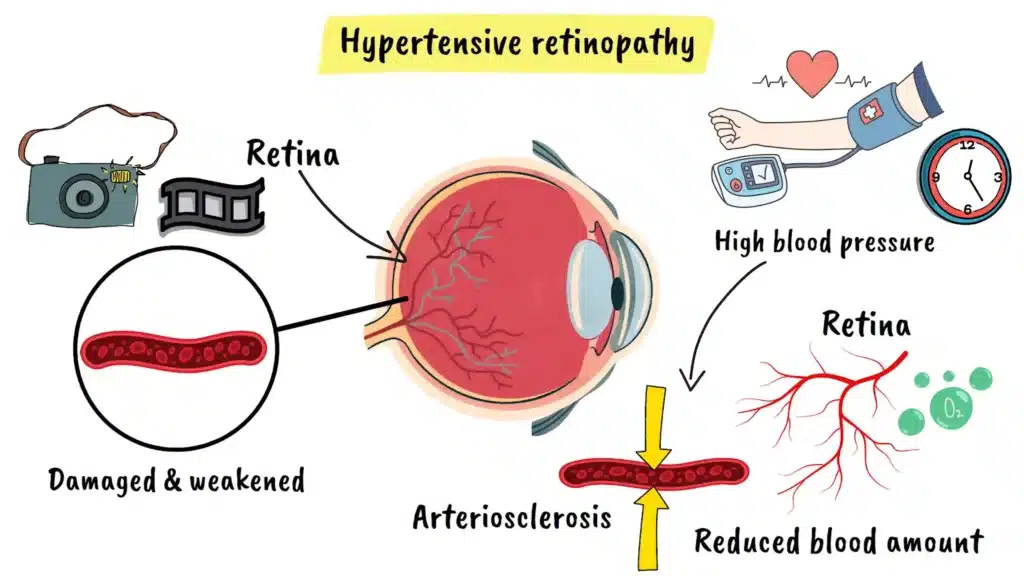
Your retina is made up of millions of tiny blood vessels that deliver oxygen and nutrients to keep your vision sharp and clear. When your blood pressure is elevated, this excessive force pushes against the walls of these small vessels day after day. The vessel walls begin to thicken and harden in a process called arteriosclerosis. This narrowing of the blood vessels reduces the amount of blood that can flow through them, and your retina starts to suffer from inadequate blood supply.
Common Symptoms of Hypertensive Retinopathy
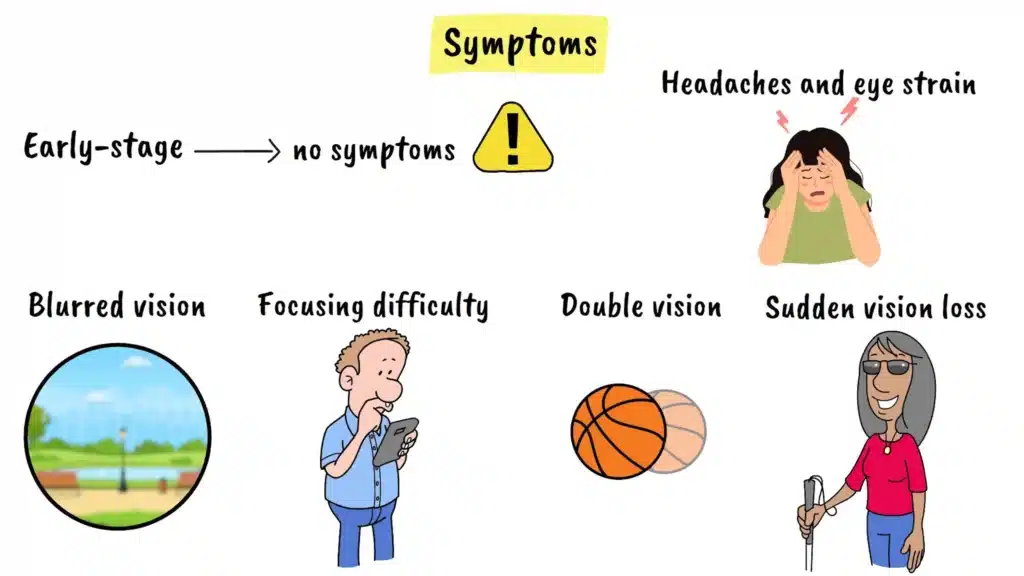
Many people with early-stage hypertensive retinopathy have no symptoms at all, which makes this condition particularly dangerous. However, as the disease progresses, symptoms may include the following.
Blurred or cloudy vision where everything appears hazy is one of the most common complaints. Some patients experience difficulty focusing on fine details or notice that their vision has become gradually less sharp over time. Double vision in one eye can also occur, where you see two images instead of one. In more severe cases, patients may experience sudden vision loss or significant changes in their visual clarity.
Headaches and eye strain are also common, particularly when blood pressure becomes dangerously elevated. These symptoms warrant immediate attention from an eye care professional.
What Causes Hypertensive Retinopathy
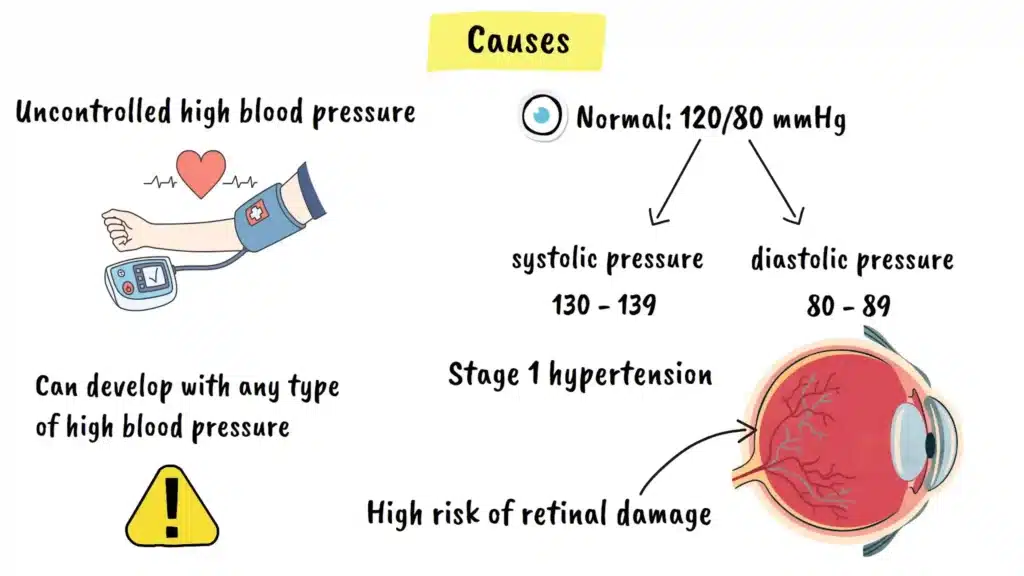
The primary cause is prolonged high blood pressure that goes uncontrolled or poorly managed. Normal blood pressure should be less than 120 over 80.
When your systolic pressure (the top number) stays between 130 and 139, or your diastolic pressure (the bottom number) stays between 80 and 89, you have stage one hypertension. If your blood pressure climbs even higher, the risk of retinal damage increases significantly.
Hypertensive retinopathy can develop in people with any type of high blood pressure, but it’s more common in those who have had hypertension for many years without proper treatment. The longer your blood pressure remains elevated, the greater the risk of permanent vision damage.
How Retinal Damage Progresses
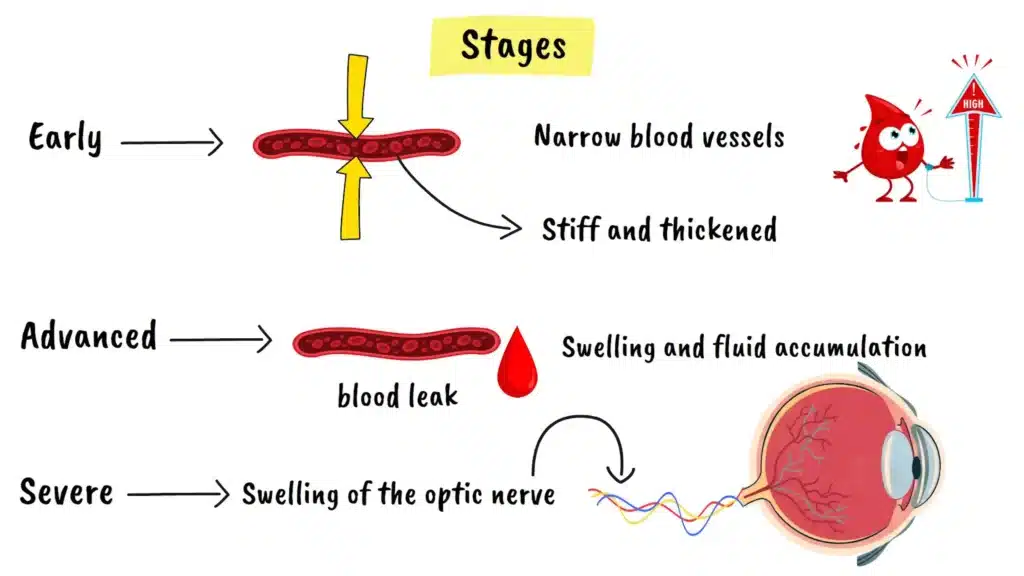
The damage to your retina progresses through distinct stages:
Earliest Stage: Your retinal blood vessels narrow as your body tries to protect itself from the excessive pressure.
Intermediate Stages: As blood pressure remains elevated, the vessel walls become stiff and thickened. In more advanced stages, blood may leak out of these damaged vessels into the retina itself, causing swelling and fluid accumulation.
Most Severe Stage: Swelling of the optic nerve occurs, which is the nerve that sends visual information from your eye to your brain. This stage poses the greatest threat to your vision.
Treatment Options for Hypertensive Retinopathy
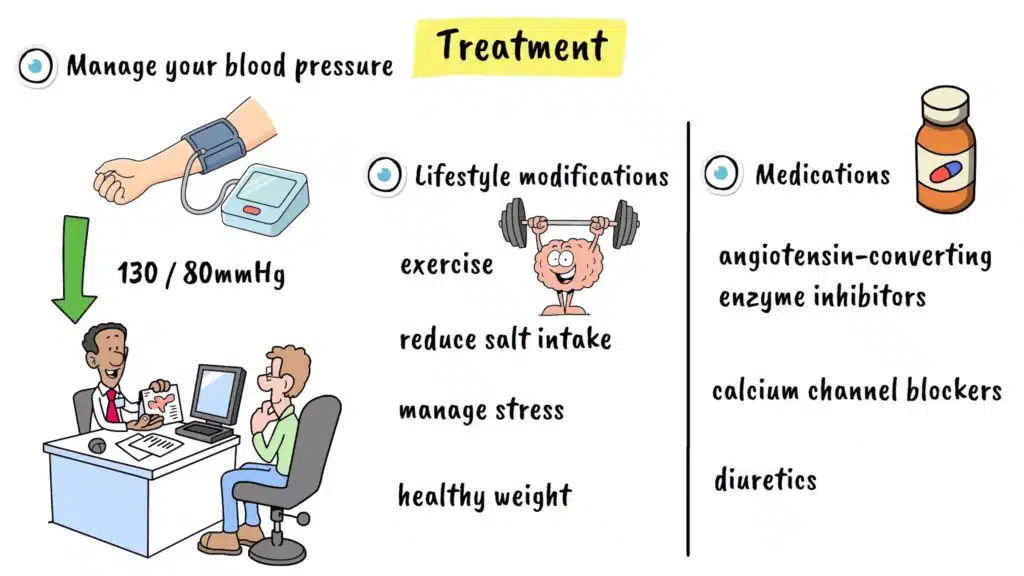
The most important treatment for hypertensive retinopathy is managing your blood pressure effectively. The goal is to reduce your blood pressure to less than 130 over 80 millimeters of mercury, ideally within two to three months. Your doctor will work with you to develop a treatment plan that may include lifestyle changes and medications.
Lifestyle Modifications include:
- Regular exercise
- Reducing salt intake
- Managing stress
- Maintaining a healthy weight
Your doctor may prescribe blood pressure medications such as:
- Angiotensin-converting enzyme inhibitors
- Calcium channel blockers
- Diuretics
In more advanced cases where significant retinal swelling or fluid accumulation has occurred, your eye doctor may recommend laser treatment to seal leaking blood vessels and prevent further vision loss. Some patients benefit from injectable medications that reduce swelling in the retina.
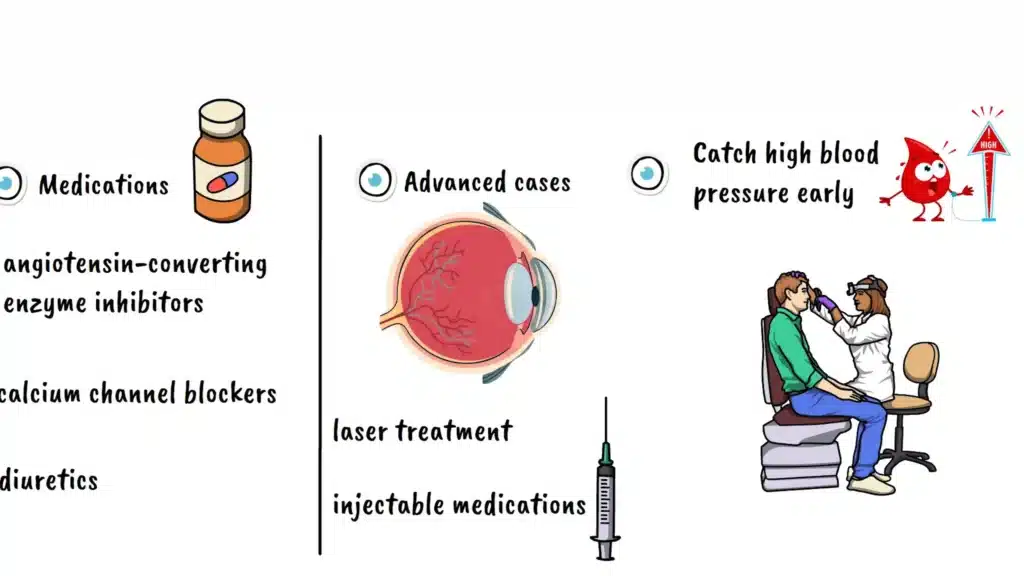
Prevention and Early Detection
The key to preventing serious complications is catching high blood pressure early and keeping it well controlled through consistent management and regular eye examinations. Don’t wait for symptoms to appear. Schedule routine eye exams at least annually, or more frequently if you have a history of high blood pressure or diabetes.