Understanding Keratoconus
Keratoconus is a progressive eye condition that affects thousands of people worldwide, causing significant changes to the structure and function of the cornea. If you’ve recently been diagnosed with keratoconus or suspect you might have this condition, understanding what it is and how it develops is the first step toward managing your eye health effectively.
What is Keratoconus?
Keratoconus is a progressive eye condition where the cornea, which is the clear dome-shaped front surface of your eye, becomes thinner and gradually bulges outward into a cone shape. To better understand this condition, think of your cornea like a clear lens that sits on the front of your eye. Normally, this lens should be perfectly smooth and round, almost like a dome that provides structural integrity to your eye’s focusing system.
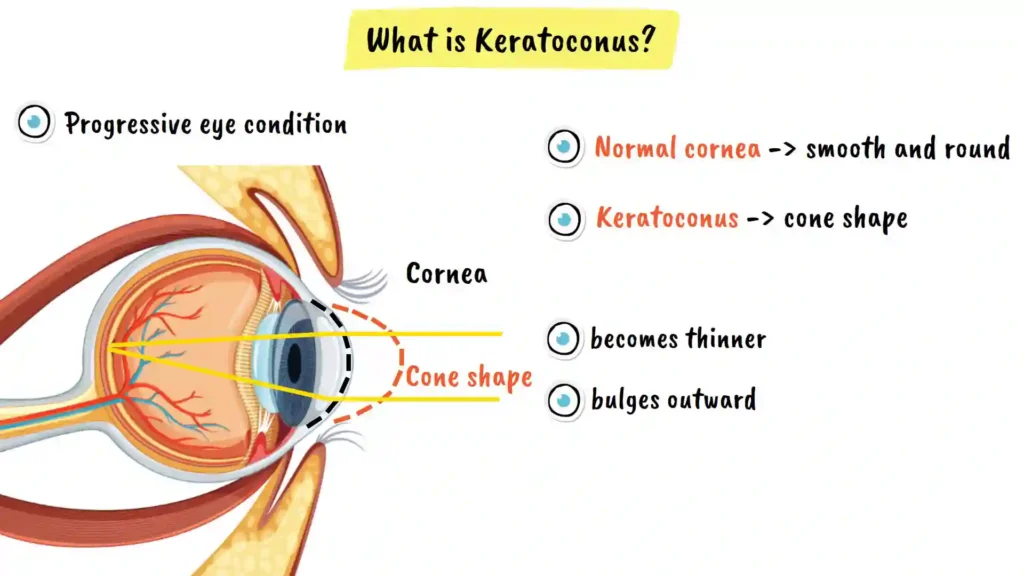
In keratoconus, however, this dome loses its strength and starts to bulge forward into a distinctive cone shape, somewhat like a pointed hat extending from the front of your eye. This deformation is what gives the condition its name: kerato means cornea, and conus means cone.
The cornea plays a crucial role in focusing light onto the retina at the back of your eye, allowing you to see clearly. When the cornea changes into this cone shape, it disrupts the way light enters your eye, leading to progressive vision problems. This distortion affects how light rays are bent and focused, resulting in the visual symptoms that characterize the condition.
Recognizing the Symptoms of Keratoconus
The symptoms of keratoconus can vary significantly from person to person, depending on the severity and progression of the condition. Being able to recognize these symptoms early is important for seeking appropriate treatment and managing the condition effectively.
Common Symptoms to Watch For
You might experience blurred or distorted vision, even when wearing glasses or contact lenses. This is one of the hallmark symptoms of keratoconus and often prompts people to seek eye care. The blurriness may fluctuate as the cornea continues to change shape.
You might notice increased sensitivity to light and glare, making it difficult to look at bright lights or drive at night. This symptom can significantly impact your daily activities and quality of life, particularly if you spend time driving or working outdoors.
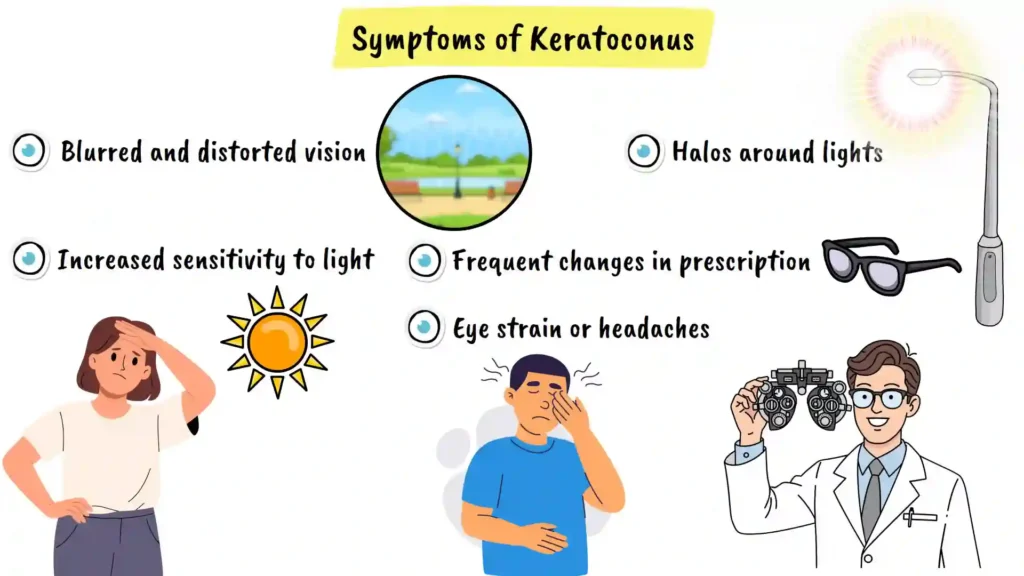
You could see halos around lights, especially at night. These halo effects occur because of the irregular corneal shape scattering light in multiple directions rather than focusing it properly on the retina.
You might also experience frequent changes in your eyeglass or contact lens prescriptions, meaning you need stronger correction every few months. This rapid change in prescription is a red flag that should prompt immediate evaluation by an eye care professional.
Some people with keratoconus experience eye strain or headaches, particularly after prolonged reading or screen time. These symptoms can become more pronounced as the condition progresses.
If you are experiencing any of these symptoms, it is important to see an eye doctor for a comprehensive evaluation. Keep in mind that these symptoms can also be caused by other eye conditions, so it is important to get a proper diagnosis from a qualified ophthalmologist or optometrist. Early diagnosis can make a significant difference in managing the condition and preserving your vision.
Understanding the Causes of Keratoconus
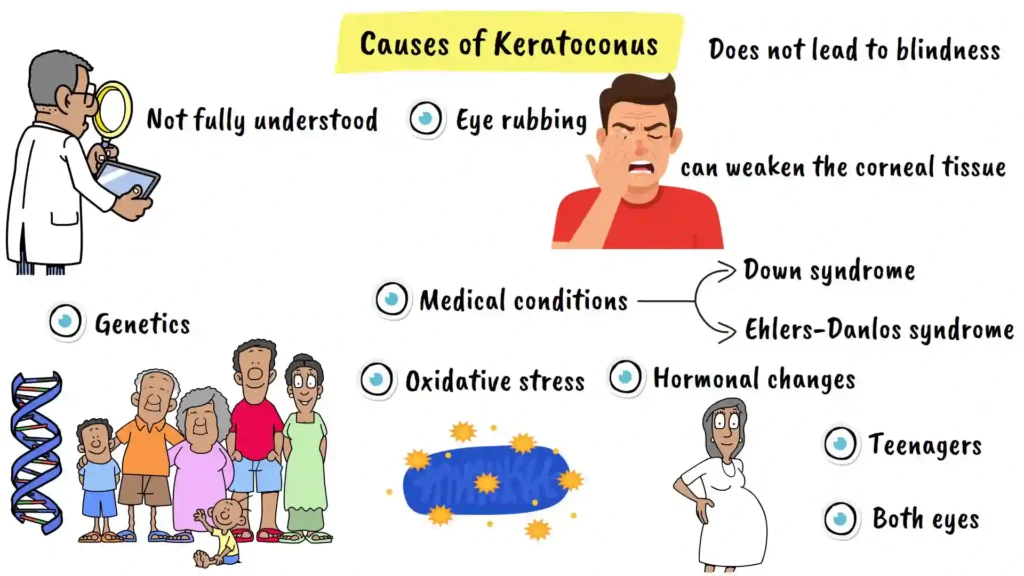
While the exact cause of keratoconus is not fully understood by medical researchers, several factors have been identified that can contribute to its development. Understanding these risk factors can help you take preventive measures and make informed decisions about your eye health.
Genetic Factors
Genetic factors play a significant role in keratoconus development. If someone in your family has keratoconus, your risk of developing it is substantially higher than the general population. This hereditary component suggests that certain genetic predispositions make the cornea more susceptible to this condition.
Eye Rubbing and Mechanical Stress
Eye rubbing is another major factor in keratoconus development. Vigorous or frequent eye rubbing, especially in people with allergies or itchy eyes, can weaken the corneal tissue over time. This mechanical stress places pressure on the cornea, potentially triggering or accelerating the cone-shaped bulging that characterizes the condition.
Associated Medical Conditions
Certain medical conditions increase the risk of developing keratoconus. These include Down syndrome and various connective tissue disorders such as Ehlers-Danlos syndrome. People with these underlying conditions should be particularly vigilant about monitoring their eye health and undergoing regular ophthalmologic screenings.
Oxidative Stress and Cellular Damage
Oxidative stress, which refers to cellular damage from harmful molecules in your body, can weaken the corneal structure over time. This cellular damage can compromise the structural integrity of the cornea, making it more vulnerable to the progressive bulging characteristic of keratoconus.
Hormonal Changes
Hormonal changes during puberty or pregnancy can also trigger or worsen keratoconus. The hormonal fluctuations during these critical life stages may affect collagen synthesis and corneal strength, potentially accelerating disease progression in susceptible individuals.
Age of Onset and Progression
The condition typically develops in teenagers or young adults and usually affects both eyes, although one eye might be more severely affected than the other. Understanding this typical pattern can help younger patients recognize symptoms early and seek appropriate care.
Importantly, it’s crucial to know that keratoconus does not lead to complete blindness, though it can significantly affect quality of life if left untreated.
Treatment Options for Keratoconus
The treatment approach for keratoconus depends on how severe the condition is and how quickly it is progressing. Fortunately, modern ophthalmology offers several effective treatment options that can help preserve vision and prevent further deterioration.
Glasses and Contact Lenses
For mild cases of keratoconus, eyeglasses can help improve vision by providing adequate optical correction. However, as the disease progresses and the cornea becomes more irregularly shaped, rigid gas-permeable contact lenses are usually required because they provide better vision correction than regular eyeglasses or soft contact lenses. These specialized lenses vault over the cone-shaped cornea, providing clearer optical correction.
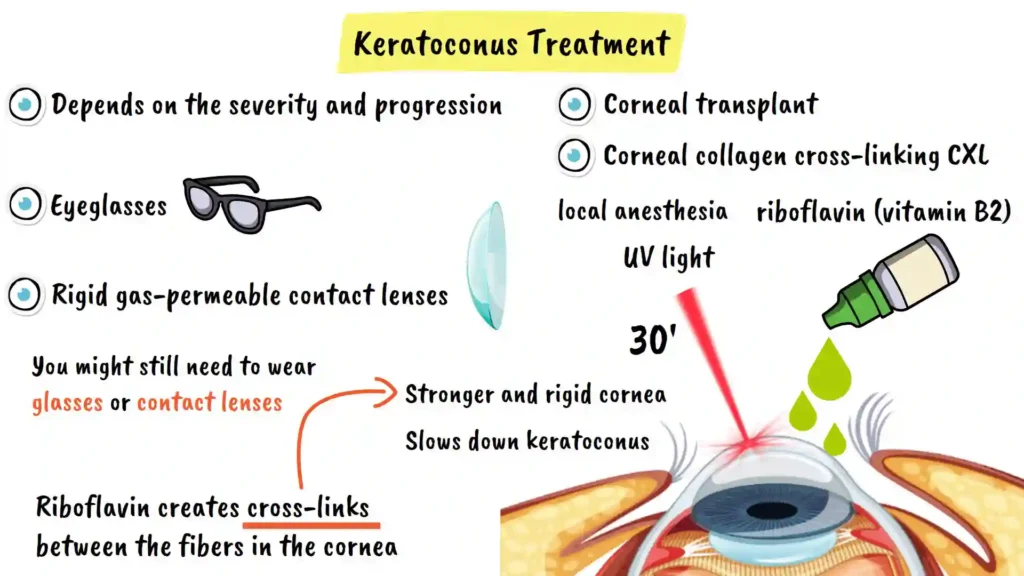
Corneal Collagen Cross-Linking (CXL)
The most effective treatment for progressive keratoconus is a procedure called corneal collagen cross-linking, often shortened to CXL. This innovative procedure has revolutionized keratoconus management by offering the possibility of halting disease progression.
In this procedure, riboflavin, which is a form of vitamin B2, is applied to the surface of your eye as eye drops. The cornea absorbs this riboflavin over a period of time. Then, ultraviolet light is directed onto your cornea for approximately 30 minutes. This ultraviolet light causes the riboflavin to create tiny cross-links or bridges between the collagen fibers in your cornea. These cross-links act like reinforcing cables, making your cornea stronger and more rigid, providing structural support to the weakened tissue.
This process stops or slows down the cone-shaped bulging, helping to prevent further vision loss and preserving your remaining visual function. The procedure is performed under local anesthesia, meaning you are awake but your eye is numbed with anesthetic drops, so you won’t experience pain during the treatment.
The entire procedure typically takes around 30 minutes, and you can usually go home the same day. Recovery is relatively quick, though you may experience some temporary discomfort and light sensitivity in the days following the procedure.
Post-Treatment Considerations
After corneal cross-linking treatment, you might still need to wear glasses or contact lenses, as the procedure is designed to stop progression rather than immediately improve vision. However, many patients appreciate that CXL prevents the need for more invasive interventions.
Corneal Transplant
In rare cases where keratoconus is very severe and other treatments have been exhausted, a corneal transplant might be necessary. In this procedure, a donor cornea replaces your affected cornea, restoring a more normal corneal shape and improving vision. While corneal transplants are highly successful procedures with good outcomes, they are typically reserved for advanced cases where other treatments have proven insufficient.
Conclusion and Next Steps
Keratoconus is a manageable eye condition when diagnosed and treated appropriately. If you suspect you have keratoconus or have recently been diagnosed with this condition, the most important step is to consult with a qualified ophthalmologist who has experience managing progressive corneal diseases.
Regular eye examinations and early intervention can make a significant difference in preserving your vision and maintaining your quality of life. With modern treatment options like corneal collagen cross-linking, many patients can effectively halt disease progression and maintain stable vision for years to come.
Don’t hesitate to reach out to an eye care professional if you’re experiencing any of the symptoms described in this guide. Your vision is precious, and early intervention is key to the best outcomes.