Imagine your eye is like a beautiful house with many different rooms, each serving a specific purpose to keep everything running smoothly. Now, what if one day the walls between these rooms started getting inflamed and swollen, making it difficult for light to pass through and causing pain throughout the entire structure? That’s essentially what happens with uveitis, a serious eye condition that affects millions of people worldwide and can threaten your vision if left untreated.
Welcome to Eye Conditions Explained, where we break down complex eye health topics using simple analogies, stories, and examples so that you can easily understand them. In this article, we’re going to explore what uveitis is, why it happens, and what puts you at risk for developing this sight-threatening condition.
Understanding the Uvea and Uveitis
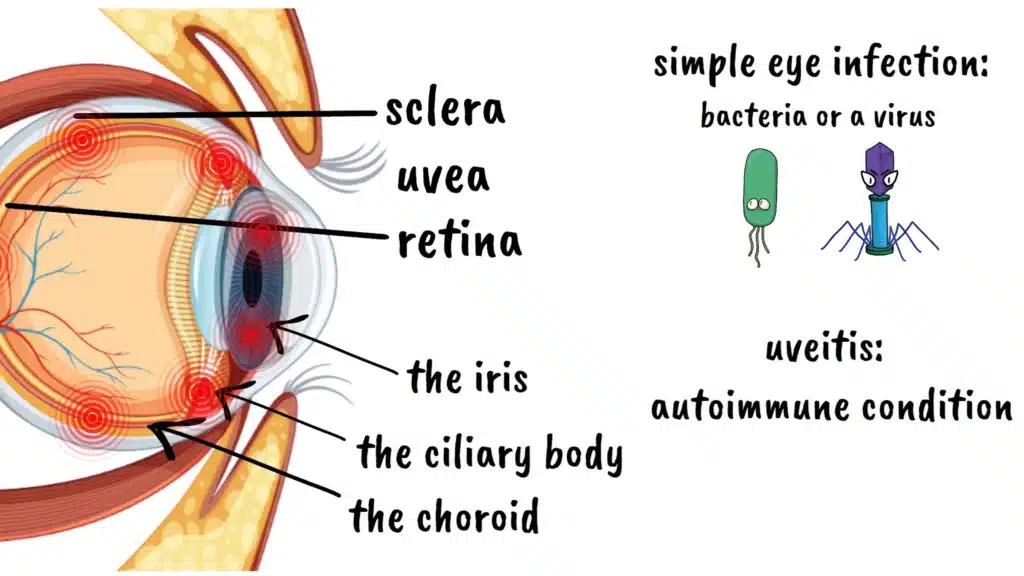
First, let’s understand what we’re dealing with. The uvea is the middle layer of your eye, sandwiched between the outer white layer called the sclera and the inner light-sensitive retina. Think of the uvea as the eye’s central heating and air conditioning system. It’s made up of three main parts: the iris, which is the colored part of your eye that controls how much light enters; the ciliary body, which changes the shape of your lens so you can focus; and the choroid, which is packed with blood vessels that supply nutrients to your retina.
When we say someone has uveitis, we’re talking about inflammation in any part of this uveal system. It’s like having your eye’s infrastructure become inflamed and irritated, similar to how your throat gets red and swollen when you have strep throat, except this is happening inside one of your most precious organs.
Uveitis as an Autoimmune Condition
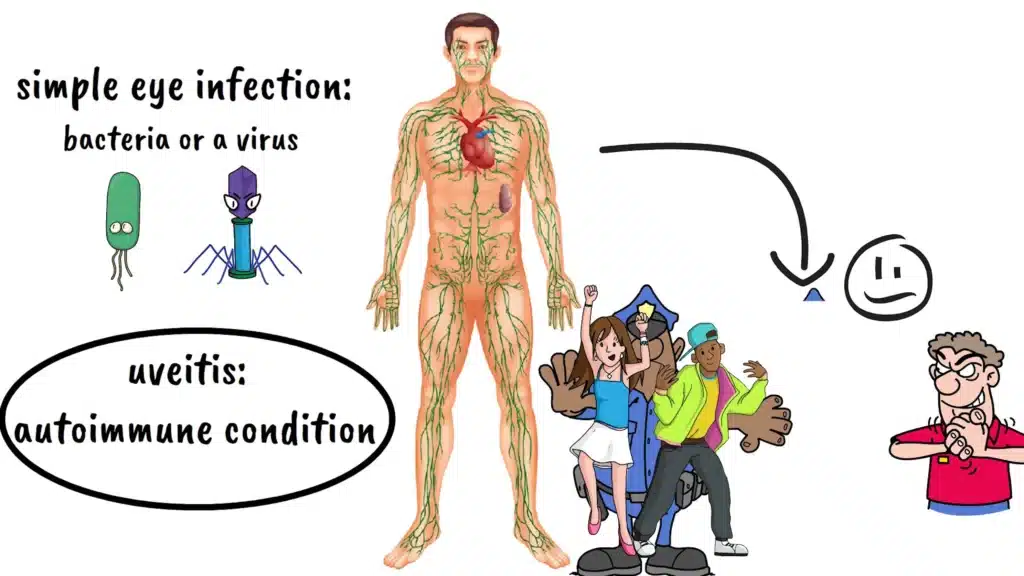
Now, here’s where uveitis gets particularly interesting and complex. Unlike a simple eye infection that might be caused by bacteria or a virus, uveitis is often what we call an autoimmune condition. To understand this, imagine your body’s immune system as an overzealous security guard at a concert. Normally, this guard does a great job keeping troublemakers out and maintaining order. But sometimes, this security guard gets confused and starts attacking the very people who belong at the concert. That’s what happens with autoimmune uveitis. Your immune system mistakenly identifies parts of your own eye as foreign invaders and launches an attack against them.
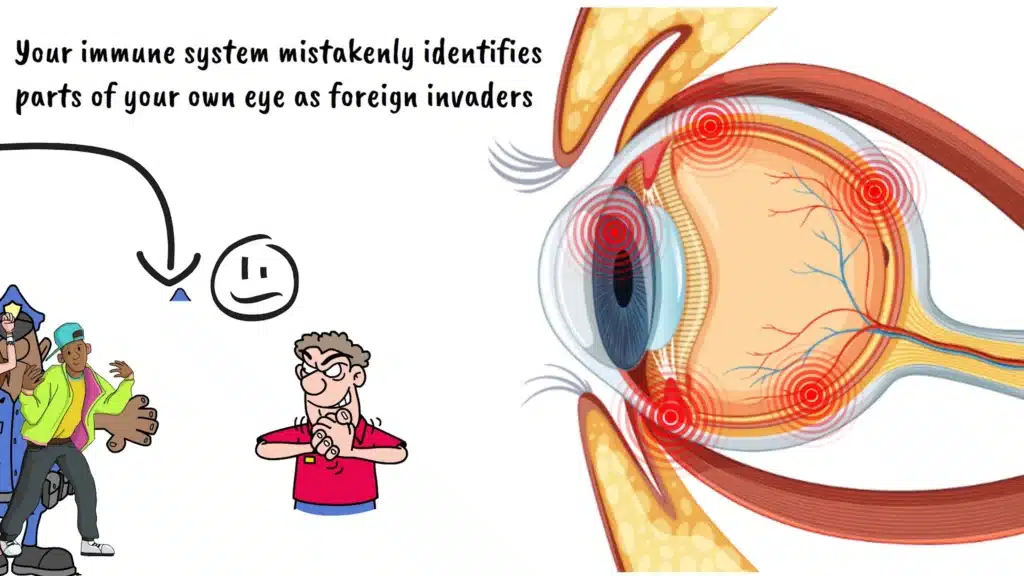
This immune system confusion can happen for several reasons. Sometimes it’s triggered by a previous infection. Your immune system fights off the infection successfully, but then gets its wires crossed and continues fighting even after the threat is gone, now targeting your eye tissue instead. Other times, it’s part of a larger autoimmune disease affecting multiple parts of your body.
Types of Uveitis
There are several types of uveitis, classified by which part of the uvea is affected.
Anterior Uveitis
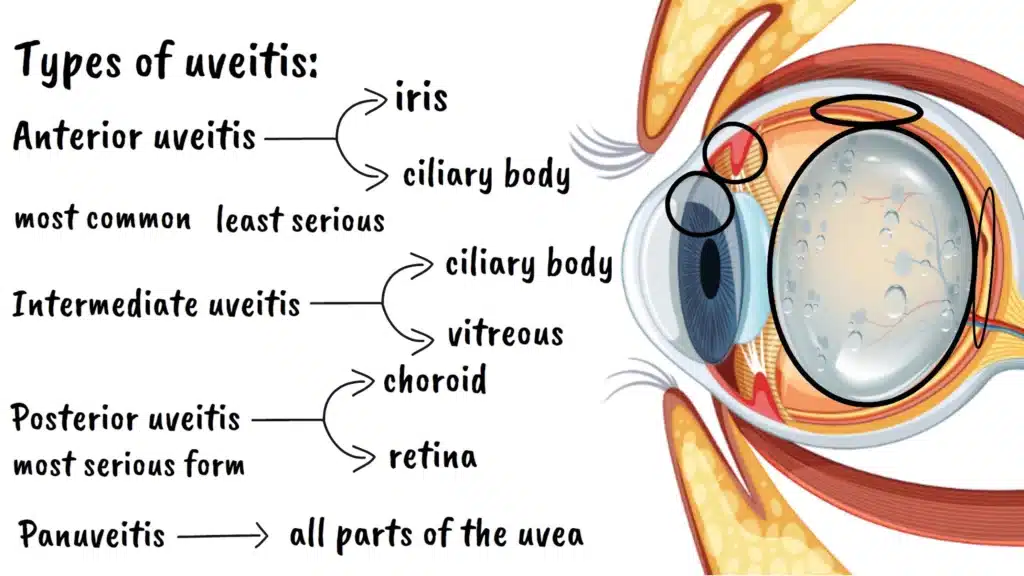
Anterior uveitis affects the front part of the eye, particularly the iris and ciliary body. This is the most common type and often the least serious. Think of it as inflammation in the front lobby of your house. It’s uncomfortable and noticeable, but not necessarily affecting the deeper structural elements.
Intermediate Uveitis
Intermediate uveitis affects the middle part of the eye, primarily the ciliary body and the gel-like substance called the vitreous that fills your eye. This is like having inflammation in the main living areas of your house. It’s more serious and potentially more disruptive to daily function.
Posterior Uveitis
Posterior uveitis affects the back part of the eye, including the choroid and often extending to the retina. This is the most serious form because it directly threatens the retina, which is like the film in a camera where images are captured. When posterior uveitis occurs, it’s like having inflammation in the most critical structural areas of your house.
Panuveitis
Then there’s panuveitis, which affects all parts of the uvea simultaneously. This is like having inflammation throughout your entire house, from the front door to the back rooms, making it the most severe and challenging form to treat.
Causes of Uveitis
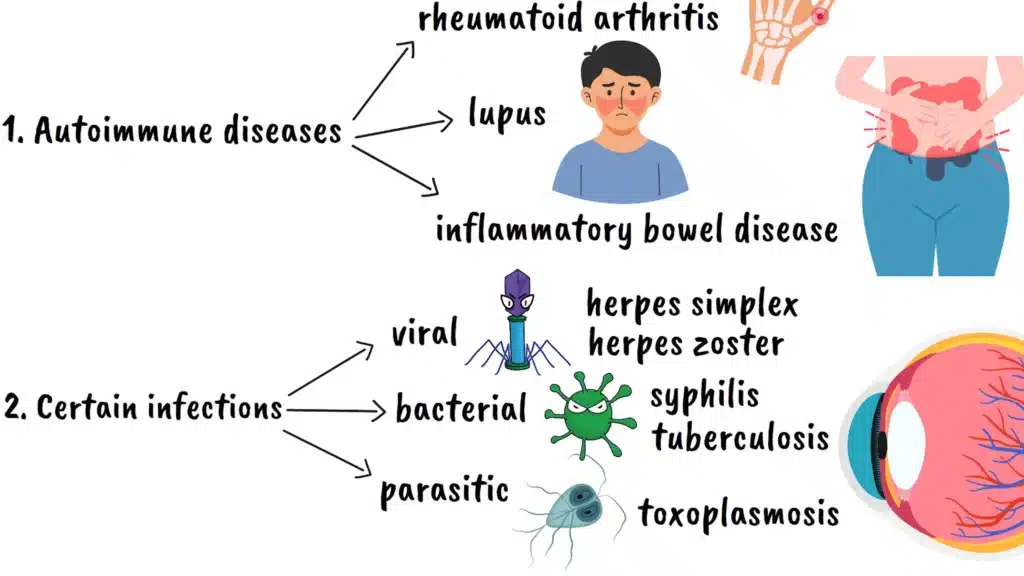
The causes of uveitis are remarkably diverse, which is part of what makes this condition so challenging to diagnose and treat. Many cases are associated with autoimmune diseases like rheumatoid arthritis, lupus, or inflammatory bowel disease. It’s as if these systemic conditions create a state of immune system hyperactivity that can spill over into the eyes.
Infections and Uveitis
Certain infections can also trigger uveitis. These include viral infections like herpes simplex or herpes zoster, bacterial infections like syphilis or tuberculosis, and even parasitic infections like toxoplasmosis. In these cases, the infection either directly invades the eye tissue or triggers an immune response that affects the uvea.
Eye Trauma and Surgery
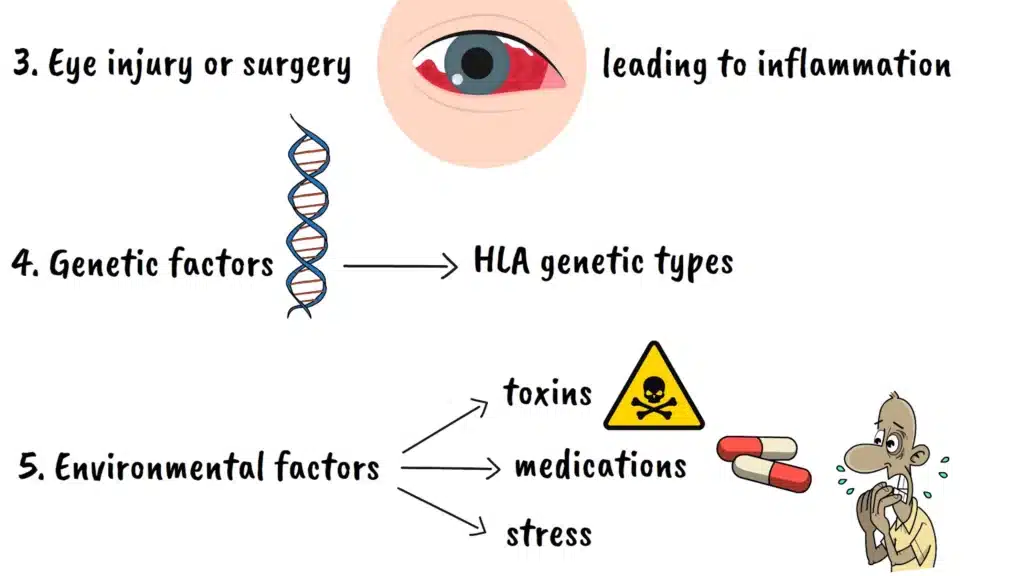
Some people develop uveitis following an eye injury or surgery. The trauma can disrupt the normal immune privilege that the eye enjoys, leading to inflammation. It’s like accidentally damaging the security system in your house, making it more vulnerable to problems.
Genetic Factors
Genetic factors also play a role in uveitis susceptibility. Certain genetic markers, particularly those involved in immune system function, can increase your risk. People with specific HLA genetic types are more prone to developing certain forms of uveitis, especially when exposed to particular triggers.
Environmental Factors
Environmental factors can contribute as well. Exposure to certain toxins, medications, or even stress can potentially trigger uveitis in susceptible individuals. It’s like having a house that’s structurally sound but becomes vulnerable when exposed to specific environmental conditions.
Why Uveitis is Concerning
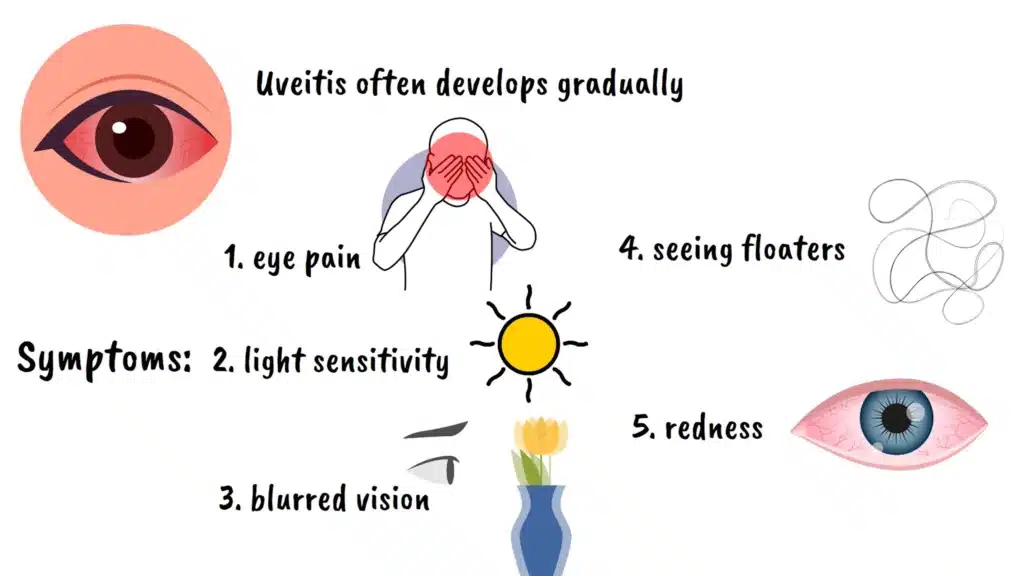
What makes uveitis particularly concerning is that it often develops gradually and can cause permanent damage before you realize something is wrong.
The symptoms can vary depending on which type you have, but common signs include eye pain, light sensitivity, blurred vision, seeing floaters, and redness. However, some forms of uveitis, particularly chronic posterior uveitis, can be essentially silent, causing progressive vision loss without obvious symptoms.
Complications of Uveitis
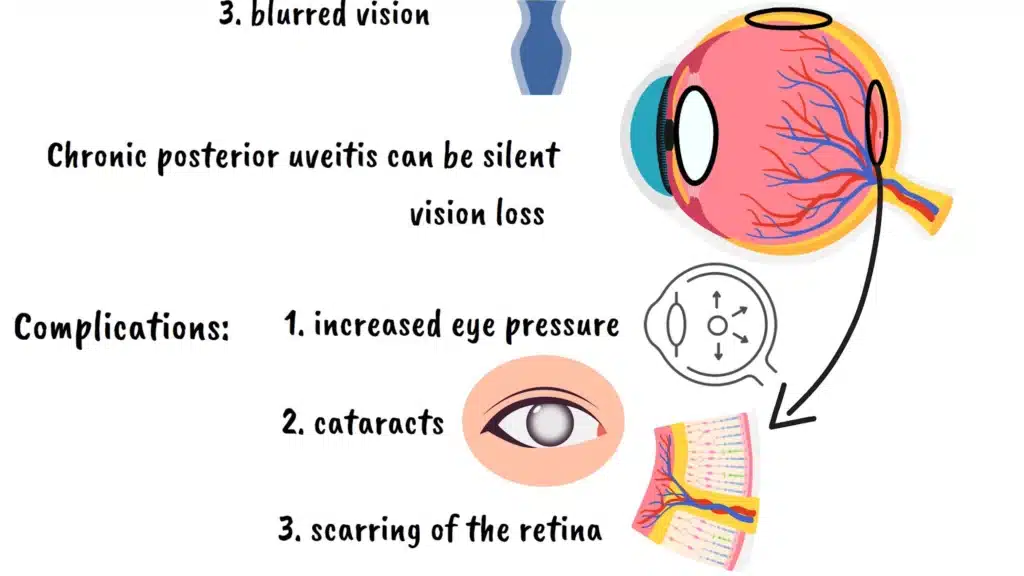
The inflammation associated with uveitis can lead to several serious complications if not properly managed. Increased eye pressure similar to glaucoma can develop when inflammation affects the eye’s drainage system. Cataracts can form when inflammation affects the lens. Most seriously, the inflammation can cause scarring of the retina or other critical eye structures, leading to permanent vision loss.
One of the most challenging aspects of uveitis is that it often tends to be a chronic, recurring condition rather than a one-time problem. Many people with uveitis will experience periods of inflammation followed by periods of remission, requiring ongoing monitoring and treatment throughout their lives.
Uveitis Diagnosis
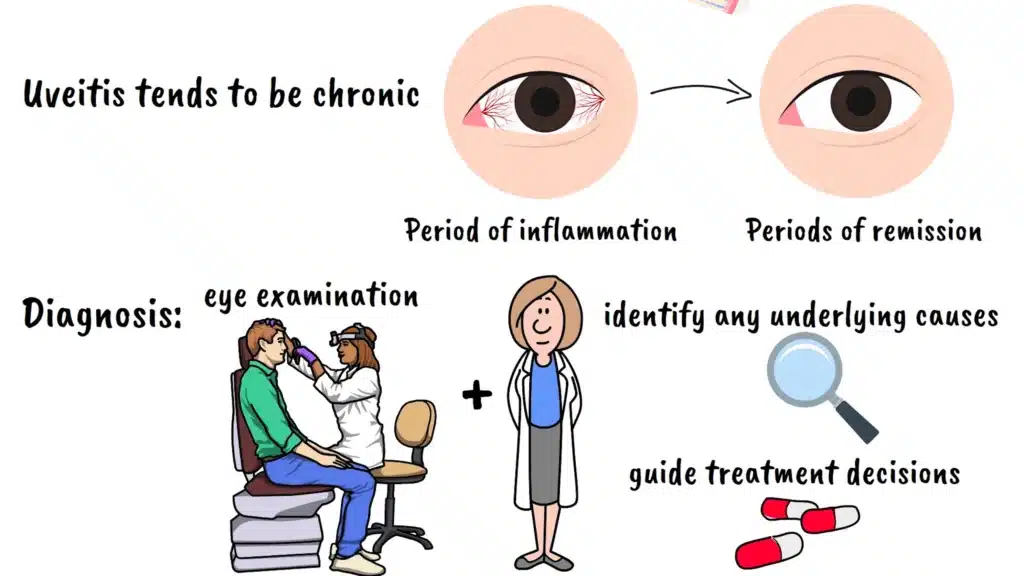
The diagnosis of uveitis requires a comprehensive eye examination by an eye care professional, often in conjunction with other medical specialists. Because uveitis can be associated with so many different systemic conditions, the diagnostic process often involves extensive testing to identify any underlying causes and guide treatment decisions.

What’s particularly important to understand is that uveitis is not contagious. You can’t catch it from someone else, and you can’t spread it to others. However, if it’s related to an underlying infection, that infection might be contagious, so proper medical evaluation is always important.
The Importance of Early Detection
The key message here is that uveitis is a serious condition that requires prompt medical attention. While it can be challenging to diagnose and treat, modern medicine offers many effective options for managing the inflammation and preserving vision. The earlier it’s caught and properly treated, the better the chances of preventing permanent damage and maintaining good vision throughout your life.



