Do your eyes feel dry, gritty, or burn after a long day at the computer? You’re not alone. More than 16 million Americans deal with dry eye syndrome, and it’s only getting worse with our screen-heavy lifestyles.
So what exactly is dry eye syndrome? Simply put, it’s when your eyes don’t produce enough tears or the right quality of tears to keep your eyes comfortable and healthy. Think of tears as your eye’s natural moisturizer and protector. When this system breaks down, everyday activities like reading, driving, or even watching TV can become uncomfortable challenges.
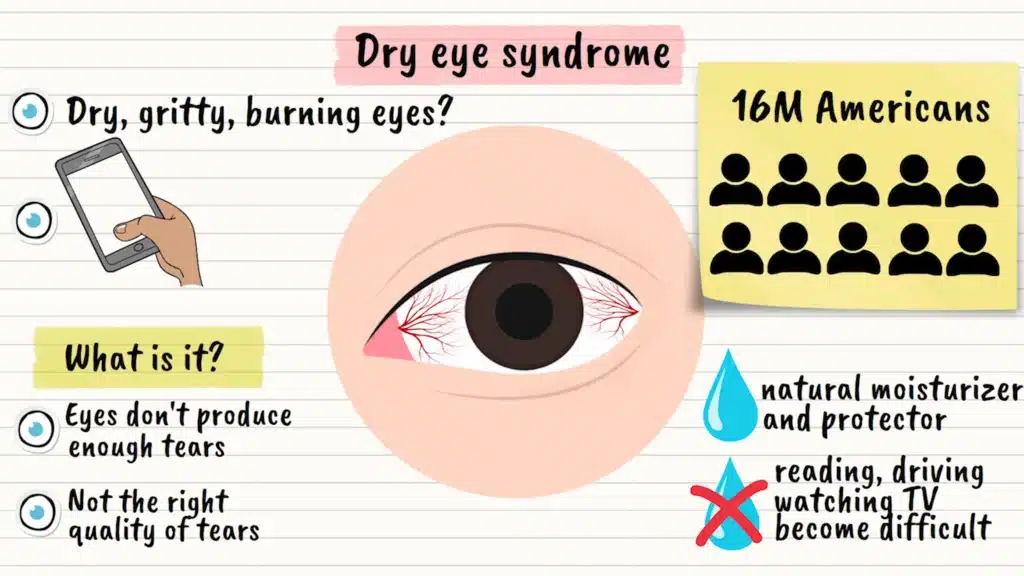

Here’s a statistic that might surprise you: between 16.7 and 50.2 million Americans currently live with dry eyes. That’s roughly one in every ten to fifteen people. Women are hit particularly hard, experiencing dry eyes about twice as often as men. And with our increasingly digital world, these numbers are only growing.
The condition isn’t just about discomfort, either. Dry eye syndrome costs the U.S. economy over 55.4 billion dollars annually, affecting productivity and quality of life for millions. But here’s the good news: understanding this condition is the first step toward managing it effectively.
That’s exactly what we’re here to do today. We’ll walk through everything you need to know about dry eye syndrome, from what causes it to how it’s treated, and most importantly, what you can do about it. Knowledge is power, especially when it comes to your eye health.
Causes of Dry Eye Syndrome
Let’s dive into what actually causes dry eye syndrome. Understanding the “why” can help you better manage or even prevent this condition.
At its core, dry eye happens for two main reasons: either your eyes don’t make enough tears, or the tears they do make aren’t good quality. Imagine your tear film as a three-layer cake. You’ve got an oily layer on top, a watery middle layer, and a mucous layer at the bottom. When any of these layers gets disrupted, problems begin.
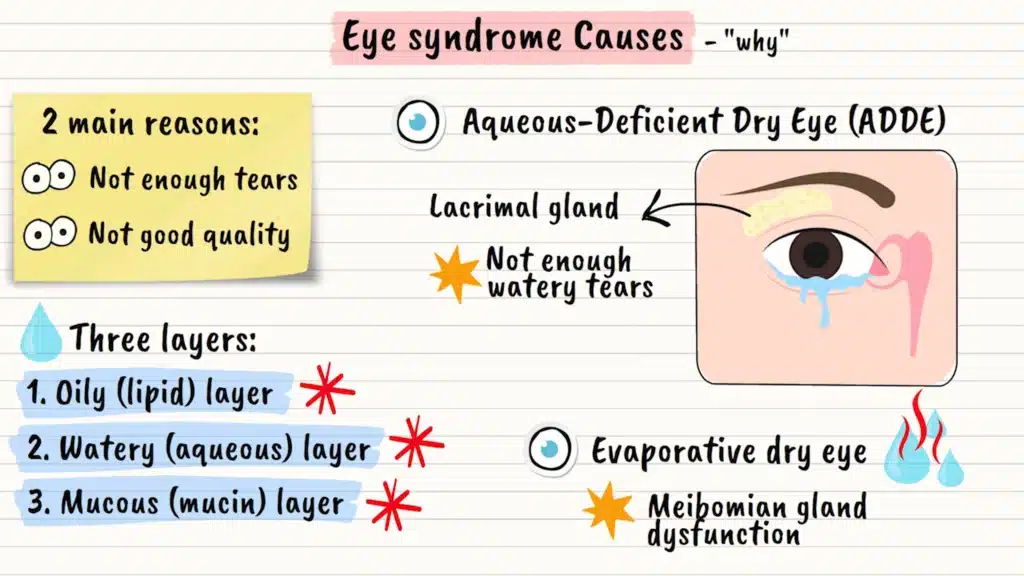
Aqueous Deficient Dry Eye
The first type is called aqueous deficient dry eye. This is when your tear glands, called lacrimal glands, simply don’t produce enough of that watery middle layer. Think of it like a faucet that’s been turned down too low. This can happen due to autoimmune conditions like Sjögren’s syndrome, where your body’s immune system mistakenly attacks your tear glands.
Evaporative Dry Eye
The second and more common type is evaporative dry eye. Here, your eyes make plenty of tears, but they evaporate too quickly. The culprit? Usually something called meibomian gland dysfunction. These tiny oil glands line your eyelids like little factories, producing the oils that keep your tears from evaporating too fast. When these glands get blocked or don’t work properly, which happens more as we age, your tears disappear like water on a hot sidewalk.
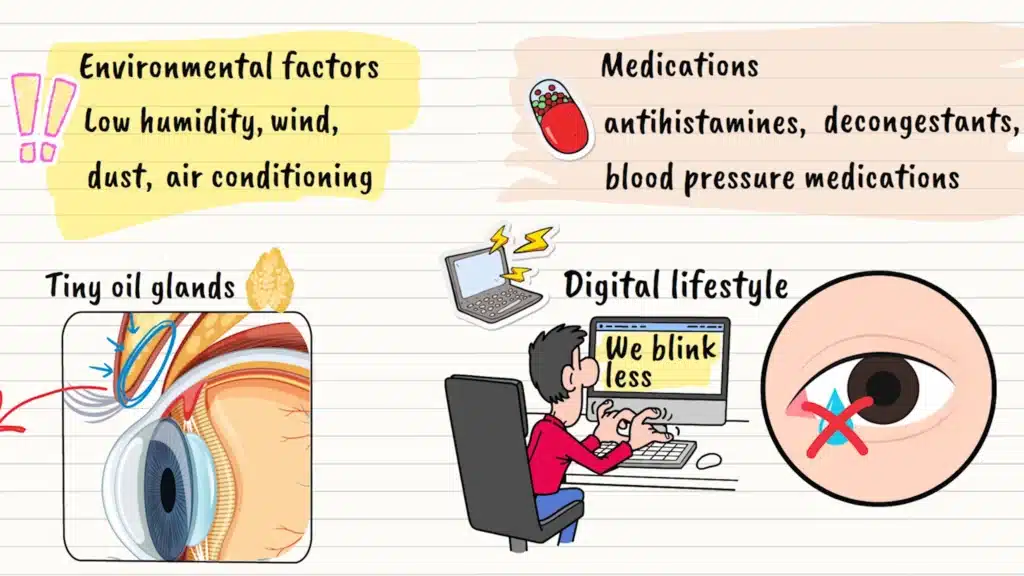
Environmental and Lifestyle Factors
Environmental factors play a huge role too. Low humidity, wind, dust, and even air conditioning can accelerate tear evaporation. It’s like trying to keep a puddle from drying up on a windy day. Certain medications, including antihistamines, decongestants, and blood pressure medications, can also reduce tear production as a side effect.
And here’s something many people don’t realize: our digital lifestyle is a major contributor. When we stare at screens, we blink less frequently and less completely, which means our tears don’t get distributed properly across the eye surface. It’s like having windshield wipers that don’t sweep often enough.
Risk Factors for Dry Eye Syndrome
Some people are simply more likely to develop dry eye syndrome than others. Let’s break down these risk factors so you know what to watch for.
Age
Age is the biggest non-modifiable risk factor. As we get older, our tear production naturally decreases, and those oil-producing meibomian glands become less efficient. If you’re over 50, your risk increases significantly. Think of it like a car that needs more maintenance as it ages. Your eyes need more attention too.

Gender
Gender plays a major role as well. Women face about twice the risk of developing dry eyes compared to men. Hormonal changes during menopause, pregnancy, or from birth control pills can all affect tear production. It’s like your body’s chemistry is constantly shifting, and sometimes your eyes get caught in the crossfire.
Medical Conditions
Certain medical conditions can set you up for dry eye problems. Autoimmune diseases like rheumatoid arthritis and Sjögren’s syndrome top this list. Diabetes is another big one. Studies show that 67 percent of diabetic patients experience dry eye symptoms. These conditions can affect the nerves that control tear production or cause inflammation that disrupts the tear film.
Lifestyle Choices
Your lifestyle choices matter too. Spending long hours in front of computers or digital devices significantly increases your risk. Contact lens wearers also face higher odds, as lenses can interfere with the natural tear film. Smoking is another modifiable risk factor that can worsen dry eye symptoms and slow healing.
Environmental factors you can often control include living in dry, windy climates or working in air-conditioned environments. Even your job matters. Farmers and outdoor workers face higher risks due to dust and wind exposure.
The good news? Many of these risk factors are things you can influence through lifestyle changes, which we’ll explore later.
Symptoms of Dry Eye Syndrome
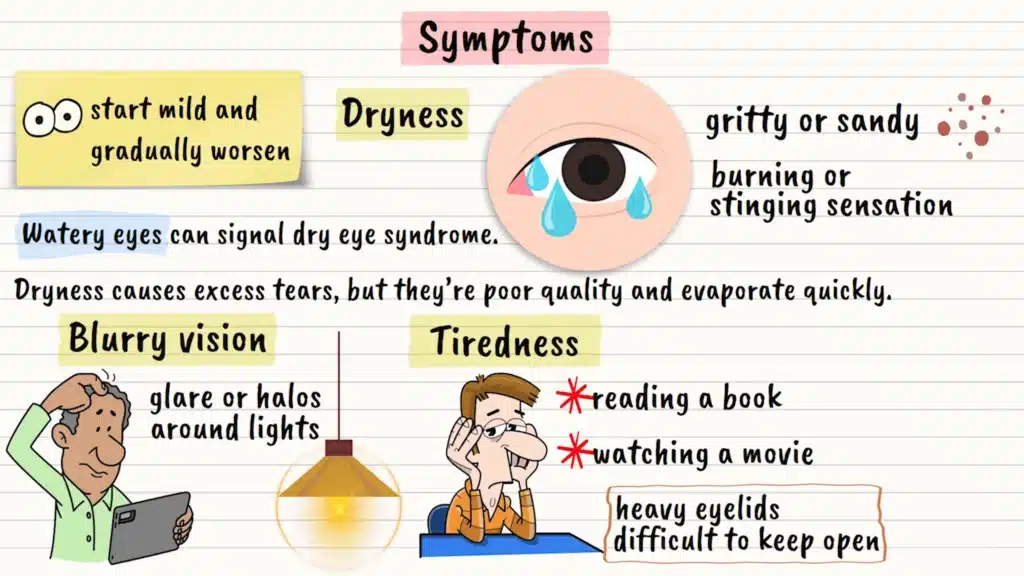
Dry eye symptoms can be sneaky. They often start mild and gradually worsen, making it easy to dismiss them as “just tired eyes” or “getting older.” Let’s walk through what to watch for.
Common Symptoms
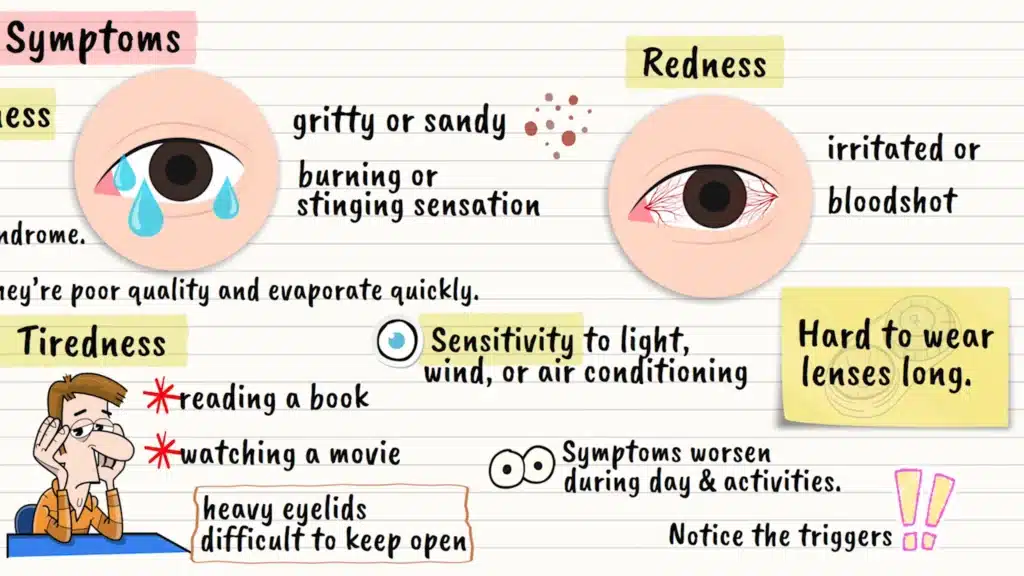
The most obvious symptom is, well, dryness. Your eyes might feel gritty or sandy, like someone sprinkled tiny particles under your eyelids. Some people describe it as a burning or stinging sensation that comes and goes throughout the day.
Here’s something that confuses many people: watery eyes can actually be a sign of dry eye syndrome. It sounds backward, but when your eyes are irritated from dryness, they sometimes overcompensate by producing too many tears. However, these are poor-quality tears that don’t stick around long enough to help.
Vision problems often creep in gradually. You might notice intermittent blurry vision, especially when reading or using a computer. Some people see glare or halos around lights, particularly at night. It’s like trying to look through a smudged window that keeps fogging up.
Your eyes might feel tired more easily than they used to. Activities that never bothered you before, like reading a book or watching a movie, suddenly leave your eyes feeling exhausted. Some people describe their eyelids as feeling heavy or difficult to keep open.
Advanced Symptoms
Redness is another common sign, though it can come and go. Your eyes might look irritated or bloodshot, especially later in the day or after screen time.
As symptoms progress, you might develop sensitivity to light, wind, or air conditioning. Contact lens wearers often find their lenses becoming increasingly uncomfortable or impossible to wear for long periods.
The key thing to remember is that these symptoms tend to worsen throughout the day and with certain activities. If you notice a pattern, like your eyes feeling worse after computer work or in air-conditioned rooms, that’s your body giving you important clues.
Diagnosis of Dry Eye Syndrome
Getting a proper diagnosis for dry eye syndrome involves several steps, but don’t worry. Most tests are quick and painless.
Let’s walk through what you can expect when you visit an eye care professional.
Medical History and Eye Exam
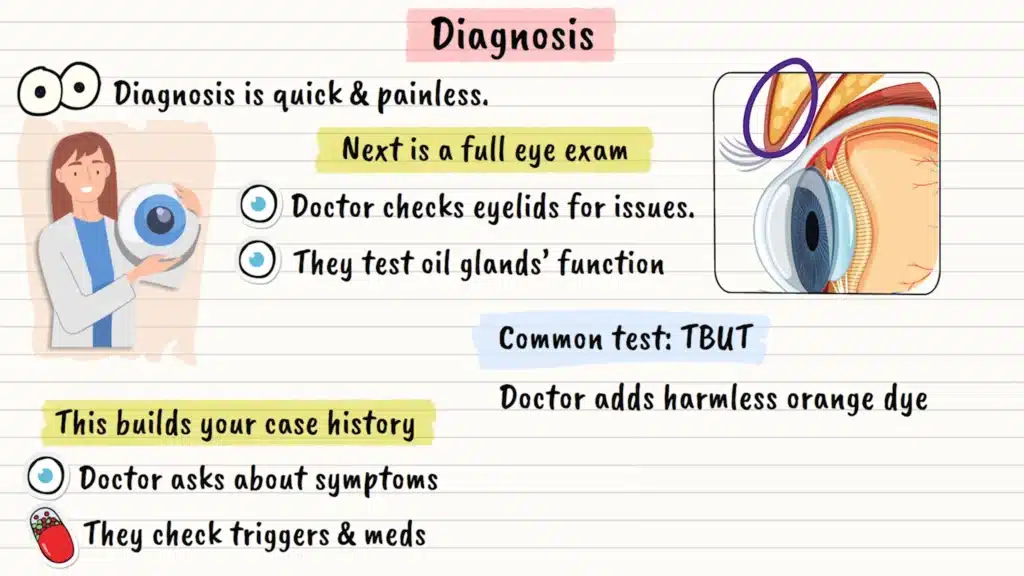
Your doctor will start with a detailed conversation about your symptoms. They’ll want to know when your eyes bother you most, what makes them feel better or worse, and what medications you’re taking. This detective work helps them understand your specific situation.
Next comes a comprehensive eye exam. Your doctor will examine your eyelids, looking for signs of inflammation or blocked oil glands. They might gently press on your eyelids to see how well your meibomian glands are functioning. Think of it as checking if those tiny oil factories are doing their job.
Tear Breakup Time Test
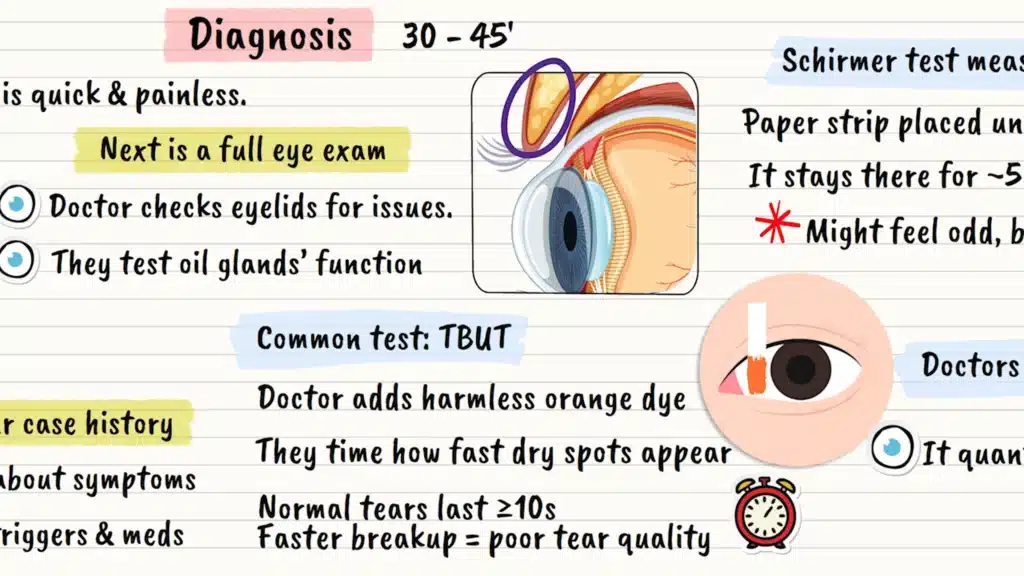
One of the most common tests is called tear breakup time, or TBUT. After placing a tiny drop of harmless orange dye in your eye, your doctor watches how long it takes for your tear film to develop dry spots. Normal tears should stay stable for at least 10 seconds. If they break up faster, it suggests your tear quality isn’t optimal.
Schirmer Test
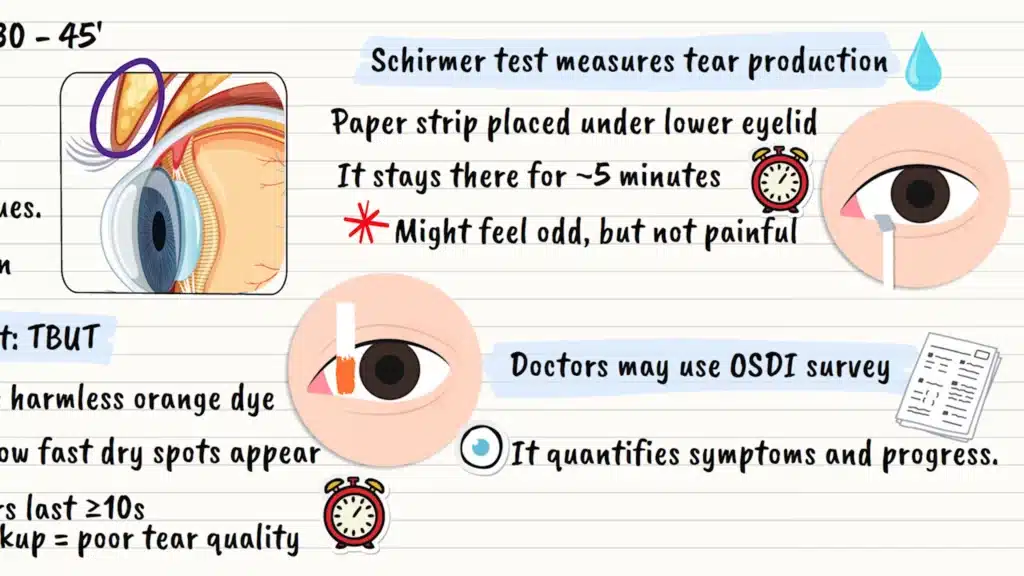
The Schirmer test measures how much tears your eyes actually produce. A small strip of paper is placed under your lower eyelid for about five minutes. It’s like a tiny measuring stick for your tears. While it might feel slightly uncomfortable, it’s not painful.
Advanced Diagnostic Tools
Some offices use more advanced technology, like tear osmolarity tests, which measure the salt concentration in your tears. Higher salt levels often indicate dry eye. There are also tests that can detect inflammation markers in your tears, giving doctors even more precise information.
OSDI Questionnaire
Many doctors will also have you fill out a questionnaire called the OSDI (Ocular Surface Disease Index). This helps quantify your symptoms and track improvements with treatment. It’s like a report card for how your eyes are feeling.
The entire diagnostic process usually takes about 30 to 45 minutes, and most tests provide immediate results.
Treatment Options for Dry Eye Syndrome
The good news about dry eye syndrome is that there are many effective treatment options available. The key is finding the right combination that works for your specific situation.
Artificial Tears
Let’s start with the most common and accessible treatment: artificial tears. These over-the-counter eye drops work like a replacement for your natural tears, providing immediate moisture and lubrication. Think of them as a drink of water for thirsty eyes. The trick is choosing the right type. Preservative-free drops are usually better if you need to use them more than four times a day.
Prescription Eye Drops
For more persistent cases, prescription eye drops can make a significant difference. Anti-inflammatory drops like cyclosporine help reduce the inflammation that often accompanies dry eye. These take several weeks to show full effects, but they can provide long-term improvement rather than just temporary relief.
Lifestyle Modifications
Lifestyle modifications can be surprisingly powerful. Simple changes like taking regular breaks from screen time can help tremendously. Follow the 20-20-20 rule: every 20 minutes, look at something 20 feet away for 20 seconds. Using a humidifier in your home or office adds moisture to the air, giving your tears less opportunity to evaporate.
Warm Compresses
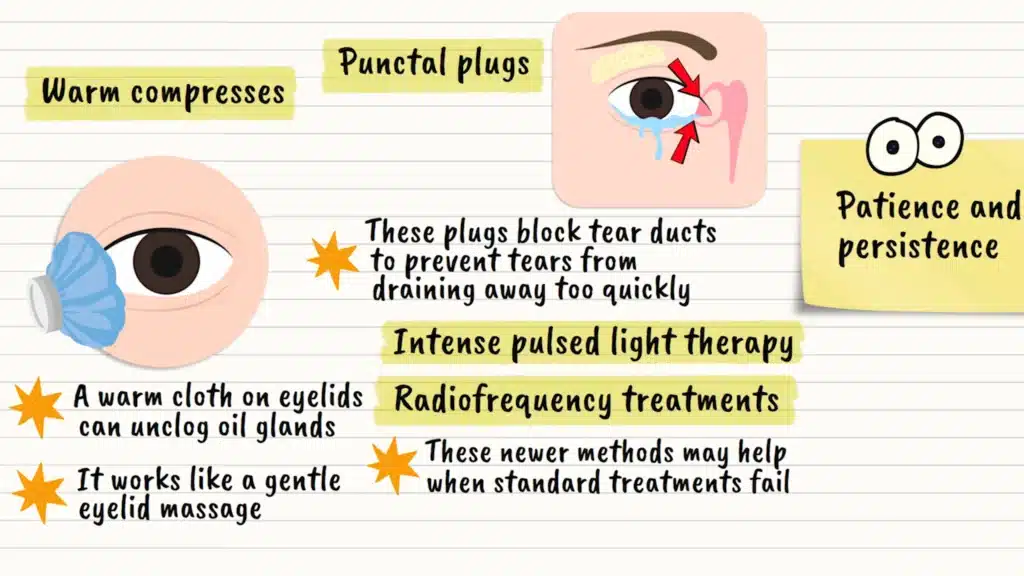
Warm compresses are another effective home treatment. Applying a warm, damp cloth to your closed eyelids for 10-15 minutes can help unclog those oil glands we talked about earlier. It’s like giving your eyelids a gentle massage to get things flowing again.
Punctal Plugs
For more severe cases, your doctor might recommend punctal plugs. These tiny devices are inserted into your tear ducts to prevent tears from draining away too quickly. Imagine putting a cork in a drain to keep the water from disappearing.
Advanced Treatments
Advanced treatments include intense pulsed light therapy and radiofrequency treatments, which can help restore proper oil gland function. These newer options show promising results for people who haven’t found relief with traditional treatments.
The key to successful treatment is patience and persistence. Most treatments take time to show their full effects, and finding the right combination might require some trial and adjustment.
Prevention and Management Strategies
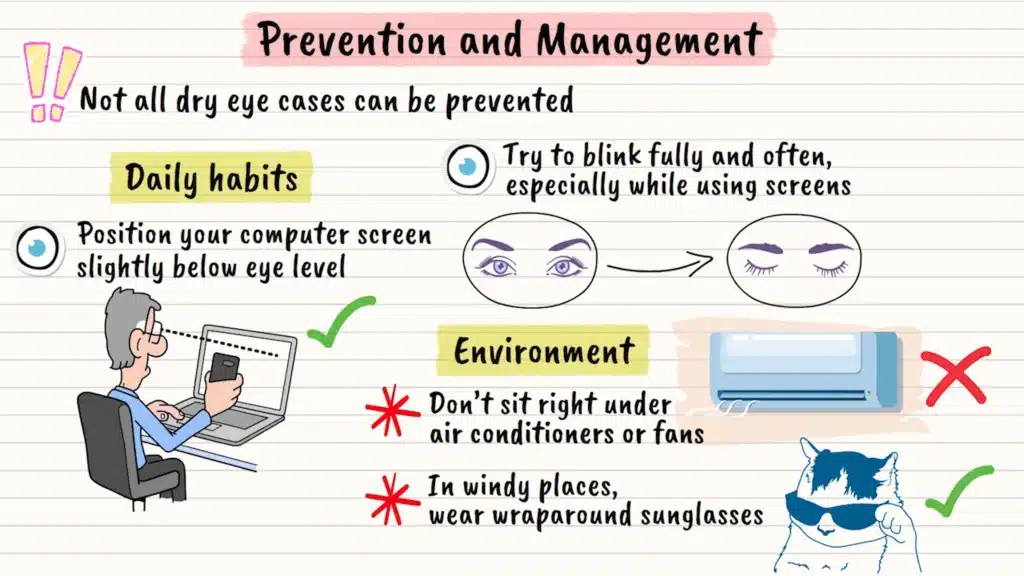
While you can’t prevent all cases of dry eye syndrome, there are many practical steps you can take to protect your eyes and manage symptoms effectively.
Daily Habits
Let’s start with your daily habits. If you work at a computer, position your screen slightly below eye level. This reduces the surface area of your eyes exposed to air, helping prevent tear evaporation. It’s like creating a natural shield for your eyes.
Blinking might seem automatic, but many of us don’t blink completely when we’re concentrating. Make a conscious effort to blink fully and frequently, especially during screen time. Think of each blink as a windshield wiper, spreading fresh tears across your eye surface.
Environmental Control
Your environment matters tremendously. Avoid sitting directly under air conditioning vents or fans. If you must be in windy conditions, consider wraparound sunglasses to create a more humid microenvironment around your eyes. It’s like creating a protective bubble for your eye area.
Diet and Hydration
Diet can play a supporting role too. Some studies suggest that omega-3 fatty acids might help with tear production, though the evidence is mixed. Staying well-hydrated throughout the day supports overall eye health. Think of it as keeping your body’s moisture reserves topped up.
Eyelid Hygiene
Regular eyelid hygiene is crucial, especially if you’re prone to blocked oil glands. Gentle cleaning with diluted baby shampoo or specialized eyelid scrubs can prevent buildup that leads to gland dysfunction. It’s like regular maintenance for your car. A little prevention goes a long way.
Medication Review
Consider your medications with your doctor. If you’re taking antihistamines, decongestants, or other drugs that can dry out your eyes, ask about alternatives or timing adjustments.
Sleep Quality
Creating good sleep habits helps too. Poor sleep can worsen dry eye symptoms, so aim for 7-8 hours of quality rest. Your eyes do important repair work while you sleep.
Regular Eye Exams
Finally, don’t ignore the importance of regular eye exams. Early detection and treatment of dry eye syndrome can prevent it from progressing to more severe stages that are harder to manage.
Impact on Daily Life
Living with dry eye syndrome affects much more than just how your eyes feel. It can reshape how you navigate your entire day. Let’s explore the real-world impact this condition can have.
Driving Challenges
Driving can become challenging, especially at night when glare from headlights creates halos and starbursts. Many people with dry eyes find themselves avoiding nighttime driving or feeling less confident behind the wheel. It’s like trying to navigate through a slightly fogged windshield that never quite clears up.
Reading and Screen Time
Reading, whether books, newspapers, or computer screens, often becomes more difficult. Your eyes might tire quickly, words might blur, or you might find yourself taking frequent breaks. Some people describe it as their eyes “giving out” after just a short time, when they used to read for hours without problems.

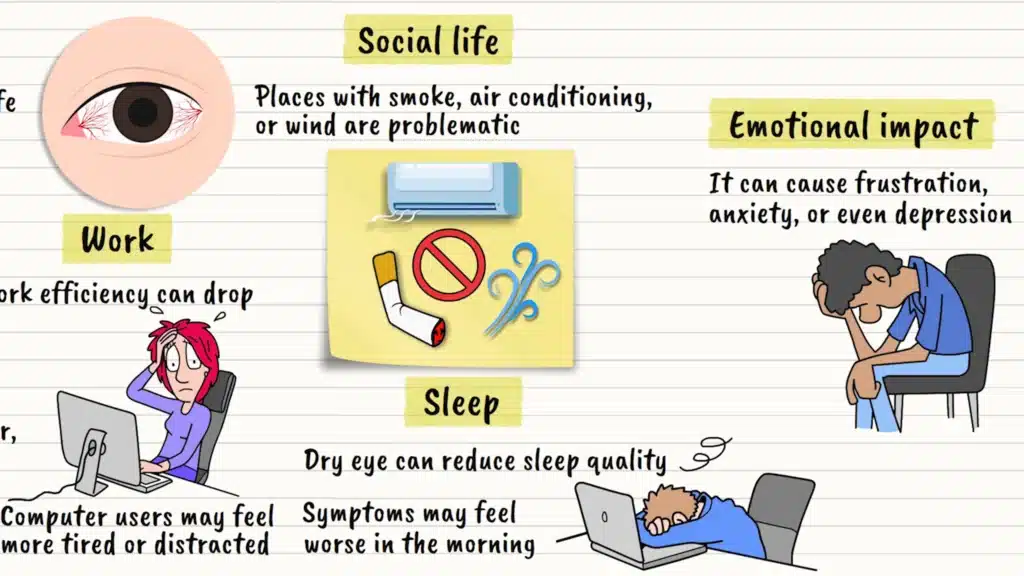
Work Productivity
Work productivity can suffer significantly. If your job involves computer use, you might find yourself less efficient or more fatigued by the end of the day. The constant discomfort can be distracting, making it harder to focus on complex tasks.
Social Impact
Social situations aren’t immune either. Smoky environments, air-conditioned restaurants, or outdoor gatherings on windy days can all trigger symptoms. Some people find themselves avoiding certain activities or locations they once enjoyed.
Sleep and Emotional Effects
Sleep quality might decline too. Dry eyes can feel worse in the morning upon waking, and severe cases might even wake you up during the night. It’s like your eyes never get a proper rest, even when the rest of your body does.
The emotional impact shouldn’t be underestimated. Chronic discomfort can lead to frustration, anxiety about activities that might trigger symptoms, and even depression in severe cases. It’s the kind of condition that touches every aspect of daily life.
Adaptive Solutions
However, there’s hope. Many people successfully adapt by using adaptive tools like computer screen filters, adjustable lighting, magnifying apps on their phones, or specialized glasses. The key is recognizing that dry eye syndrome is a legitimate medical condition that deserves attention and treatment, not something you just have to “live with.”
Current Research and Future Developments
The field of dry eye research is advancing rapidly, bringing hope for better treatments and even potential cures in the future.
The Gut-Eye Connection
Scientists are currently exploring the role of the gut-eye connection. Emerging research suggests that the bacteria in our digestive system might influence eye health in ways we’re just beginning to understand. It’s like discovering a hidden highway between two parts of your body that were thought to be unconnected.
Gene Therapy
Gene therapy represents another exciting frontier. Researchers are investigating ways to actually restore the function of damaged tear glands and oil-producing cells. Think of it as potentially giving your eyes a repair manual written in their own language.
Advanced Diagnostic Tools
Advanced diagnostic tools are also in development. New technologies promise to detect dry eye syndrome earlier and more accurately than current methods. Imagine having a test that could predict dry eye problems before you even experience symptoms.
Nanotechnology
Nanotechnology is opening doors to more effective drug delivery systems. Scientists are working on tiny particles that could deliver medication directly where it’s needed in the eye, potentially making treatments more effective with fewer side effects.
Systemic Health Connections
There’s also growing research into the connection between dry eye syndrome and other health conditions. Studies are revealing links with metabolic syndrome, diabetes, and autoimmune diseases, which could lead to more comprehensive treatment approaches.
Stem Cell Therapy
Stem cell therapy is another area showing promise. Early research suggests that stem cells might be able to regenerate damaged tear glands or restore proper oil gland function. While still in experimental stages, this could represent a true cure rather than just symptom management.
The good news is that current treatments continue to improve too. New formulations of artificial tears, better anti-inflammatory medications, and refined surgical techniques are making life better for dry eye patients right now, while we wait for these future breakthroughs.
Conclusion
We’ve covered a lot of ground today, from the basic mechanics of how dry eye syndrome develops to the cutting-edge research that might change everything in the years ahead.
Here are the key takeaways to remember: Dry eye syndrome is incredibly common, affecting millions of people worldwide. It’s not just an inconvenience. It’s a legitimate medical condition that can significantly impact your quality of life. The good news is that it’s also very treatable, especially when caught early.

Whether your dry eyes stem from too much screen time, hormonal changes, medical conditions, or simply getting older, there are effective solutions available. From simple artificial tears to advanced therapies, the treatment toolkit keeps growing.
Remember that small changes can make a big difference. Taking screen breaks, using a humidifier, wearing wraparound sunglasses in windy conditions, and practicing good eyelid hygiene are all simple steps that can provide real relief.
Most importantly, don’t ignore persistent eye discomfort. If your eyes regularly feel dry, gritty, or tired, or if your vision seems less clear than it used to be, it’s time to talk to an eye care professional. Early intervention can prevent symptoms from worsening and help you maintain the clear, comfortable vision you deserve.
Your eyes work hard for you every day. They deserve the same attention and care you’d give any other important part of your body. With the right knowledge, treatment, and ongoing care, you can keep enjoying all the visual experiences that make life rich and meaningful.
Don’t let dry eye syndrome dim your world. Take action, stay informed, and remember: clearer, more comfortable days are absolutely within reach.



