A staphyloma is a structural weak spot in the wall of the eye where the tissue becomes thin and bows outward, creating a localized “bulge” of the eyeball. It matters because the bulge can distort the eye’s optics, stress delicate retinal tissue (especially in high myopia), and—depending on location—raise the risk of long-term vision problems or surface fragility.
What is Staphyloma?
A staphyloma is an abnormal outward protrusion of the eye wall that happens when the sclera (the white outer coat) or cornea (the clear front window) becomes weakened and thinned, allowing the underlying darker layers to show through. Because the deeper pigmented tissues can be visible through the thin area, a staphyloma may look darker than the surrounding white of the eye.
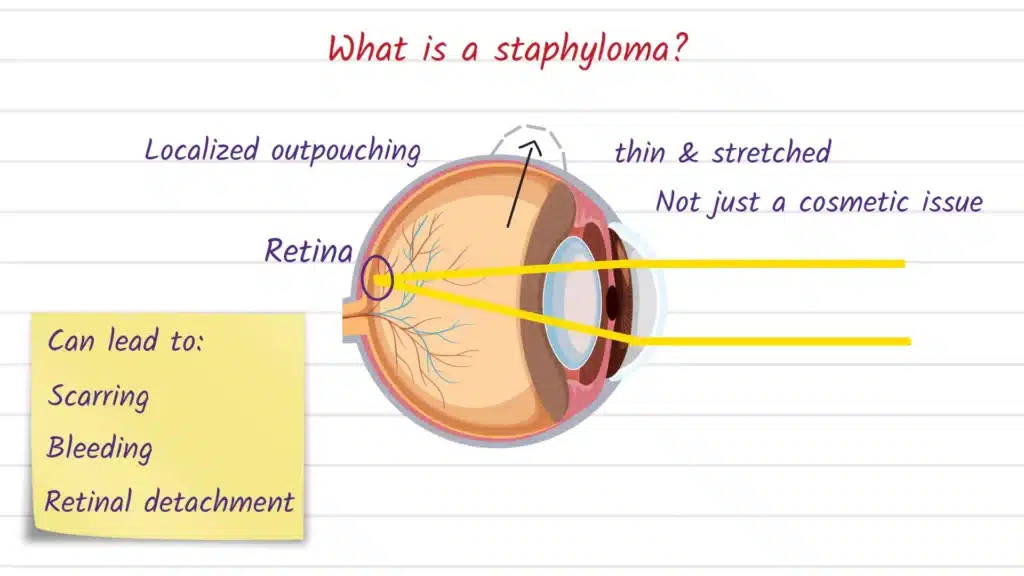
Doctors often describe staphylomas by where they occur, because location strongly influences symptoms, monitoring, and potential complications.
Common location-based types (patient-friendly overview):
| Type | Where it is | Why it matters most |
|---|---|---|
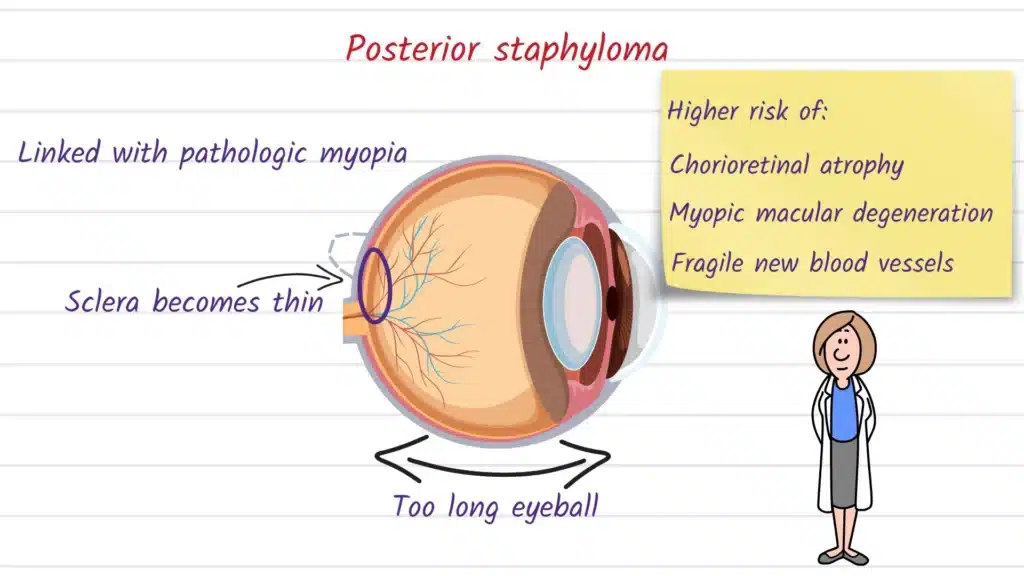
| Posterior staphyloma | Back of the eye (posterior pole), near the macula/optic nerve region | Often linked to pathologic/high myopia and associated with higher risk of myopic maculopathy and worse visual prognosis. |
| Anterior (scleral or sclerocorneal) staphyloma | Front of the eye (near cornea/limbus/sclera) | Can be a visible bulge; tissue may be very thin and fragile, sometimes following trauma or infection. |
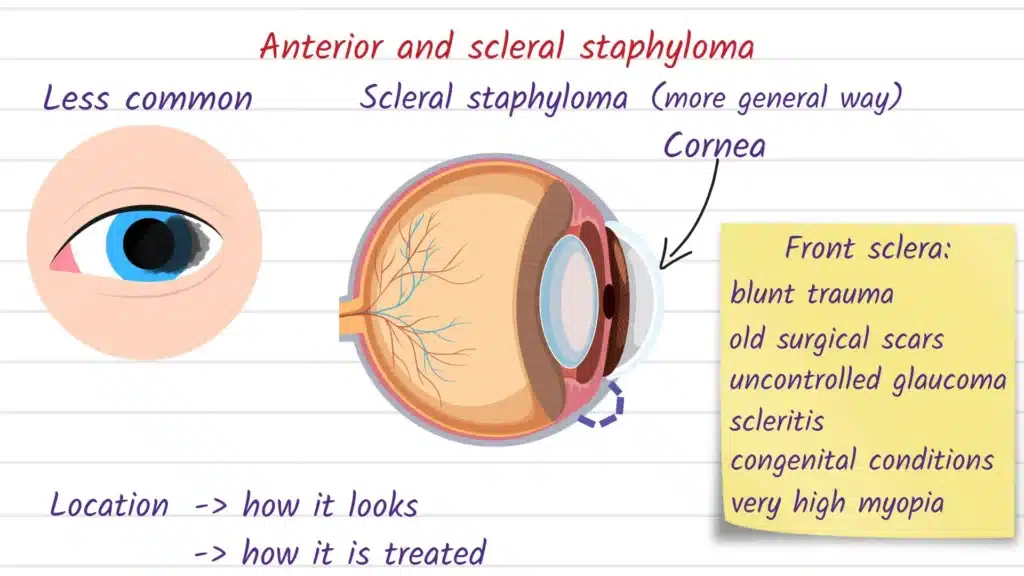
Causes and Risk Factors
Staphyloma formation is most commonly discussed in the setting of myopic eye stretching, where a longer-than-average eyeball can gradually thin and expand, predisposing the wall to outpouching. Posterior staphyloma, in particular, is widely described as a key feature of pathologic myopia and is used to help distinguish “simple” myopia from myopia with sight-threatening structural changes.
Other causes are typically conditions that damage or weaken the sclera or cornea over time, such as significant trauma or infection, which can disrupt the eye wall and make that region more vulnerable to thinning later on. In real-world practice, “risk factors” often overlap (for example, a highly myopic eye that also had prior surgery or inflammation), so your clinician considers your full eye history—not just one trigger.
Common Signs and Symptoms
Symptoms vary widely because a staphyloma can involve the back of the eye (affecting central vision) or the front surface (affecting comfort and shape). Some people—especially with posterior staphyloma—notice gradual blur or distortion as macular complications develop, while others may have few symptoms and discover the finding during imaging for high myopia.
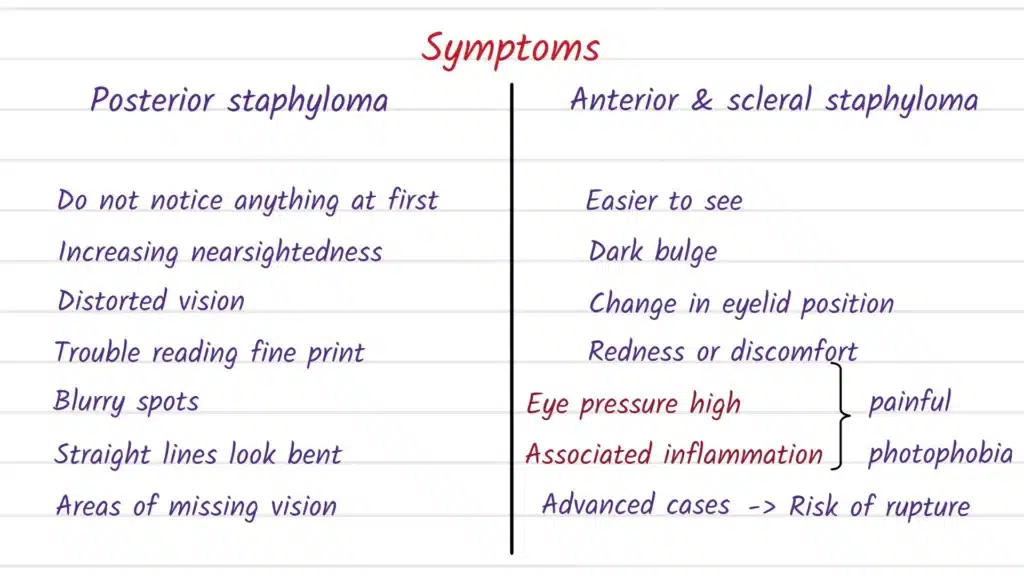
With anterior scleral staphyloma, the most obvious sign can be a dark, cyst-like or dome-shaped protrusion on the front of the eye, sometimes appearing long after an injury. Because the wall can become extremely thin in that area, doctors treat it as a structural problem (not just a cosmetic change), especially if there is discomfort, irregular astigmatism, or concern about vulnerability to further trauma.
How the Condition is Diagnosed
Diagnosis starts with a comprehensive eye exam, but imaging is what “maps” the shape and extent of the bulge and helps link eye-wall shape to retinal health. For posterior staphyloma in pathologic myopia, modern imaging and classification approaches frequently rely on advanced OCT techniques (including swept-source OCT in many research and specialty settings) to better visualize the posterior contour.
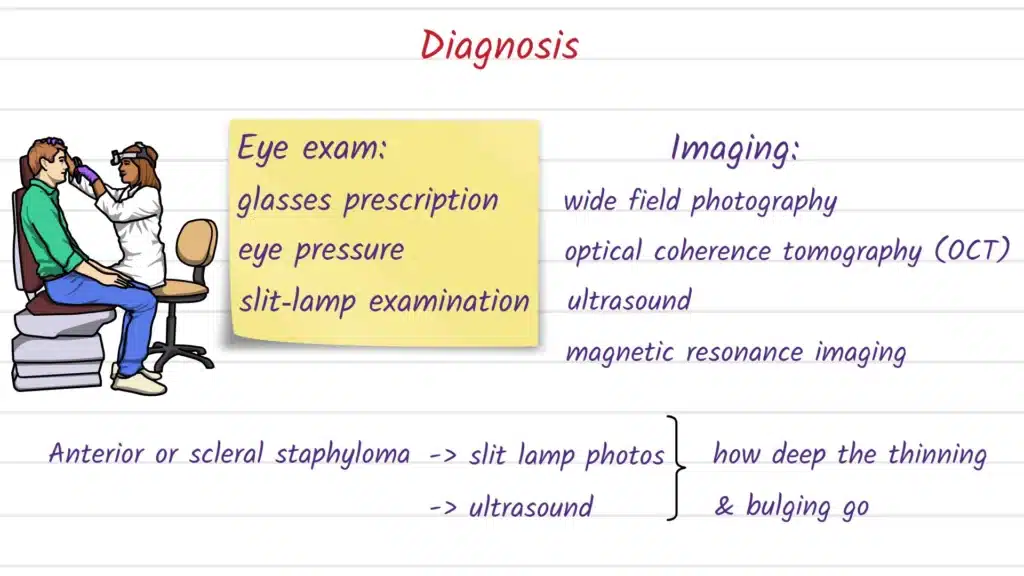
Newer quantification methods can also help describe where the posterior bulge is and how severe it appears in 3D; for example, automated posterior scleral topography approaches have been studied to visualize and quantify staphyloma location/severity and relate geometric measures to traction-related macular changes. For suspected anterior scleral staphyloma, ultrasound biomicroscopy (UBM) may be used to evaluate the cyst-like protrusion and its relationship to deeper structures, as described in case-based clinical reporting.
Treatment Options Explained (non-prescriptive, informational)
Treatment depends on the location (posterior vs anterior), the underlying cause (often high/pathologic myopia vs prior trauma/infection), and whether there are complications affecting vision, comfort, or eye integrity. There is not a simple medication that “shrinks” a staphyloma back to normal—care is typically aimed at monitoring and protecting vision, and managing complications when they arise.
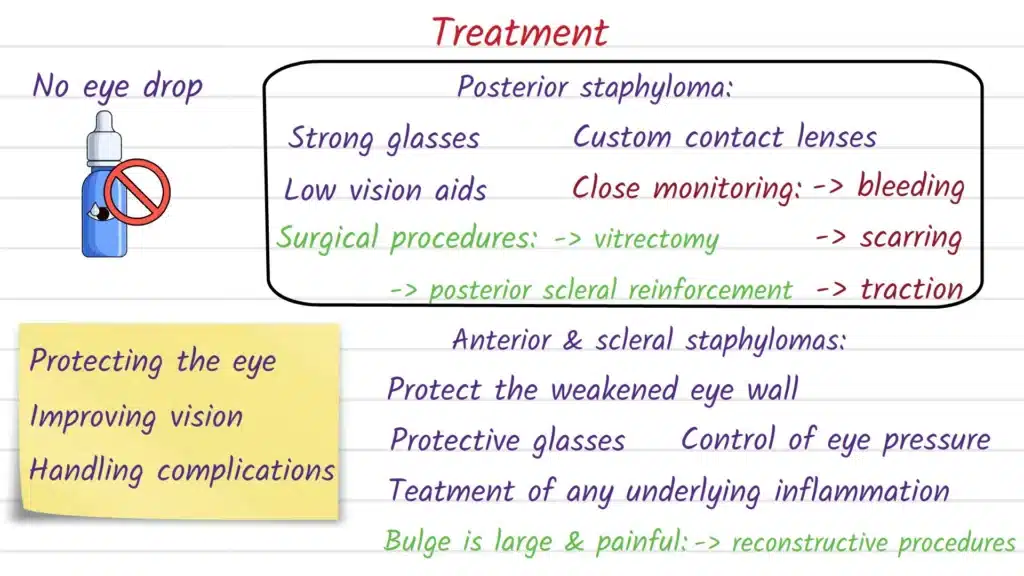
Posterior staphyloma (often with pathologic myopia):
Posterior staphyloma has been associated with more severe myopic maculopathy and worse visual prognosis in highly myopic eyes, so clinicians often focus on careful follow-up and timely detection of macular complications. In specialty retina care, the clinical conversation often centers on the retina and macula findings (atrophic, tractional, or neovascular changes) rather than the staphyloma alone.
Anterior scleral/sclerocorneal staphyloma:
When an anterior staphyloma is large, symptomatic, cosmetically troubling, or structurally risky, surgical approaches may be considered to remove abnormal protruding tissue and reinforce the area with a patch graft (for example, a scleral patch graft has been described in trauma-associated giant anterior scleral staphyloma). More complex corneoscleral reconstructive procedures—such as staged penetrating sclerokeratoplasty techniques—have been reported for advanced acquired anterior staphyloma to provide “tectonic” support (structural stability), though these can carry significant risks and may require more than one operation.
Because procedures for severe anterior staphyloma can involve complications like graft rejection/failure and secondary glaucoma (among others), treatment decisions are individualized and typically handled by cornea/anterior segment specialists.
Possible Complications if Left Untreated
Complications depend on the type and severity. In posterior staphyloma associated with high/pathologic myopia, the presence of posterior staphyloma has been linked with a higher risk of myopic maculopathy and worse visual prognosis, especially when macular involvement is present.
In advanced anterior staphyloma, the main concern is the eye’s structural integrity and surface stability, because the weakened area may be thin and prone to problems that sometimes require high-risk reconstructive surgery. Even when the goal is comfort and globe preservation (rather than vision improvement), the condition can still be medically significant due to the complexity of management and the possibility of multiple procedures.
Prevention and Risk Reduction (if applicable)
Not every staphyloma is preventable, especially when it is driven by long-term remodeling in pathologic myopia or results from unavoidable trauma. Still, risk reduction often focuses on addressing modifiable contributors to scleral/corneal weakening—most importantly, preventing eye injuries and seeking prompt care for serious eye infections or inflammation, since these can disrupt eye-wall structure and predispose to thinning.
If you have high myopia, the most practical “prevention” strategy is ongoing surveillance: regular, appropriately timed eye exams with imaging when indicated, because posterior staphyloma is clinically important in pathologic myopia and correlates with more severe macular disease in research populations.
When to See an Eye Doctor
Seek an eye exam soon (and urgently if symptoms are sudden or severe) if you have high myopia and notice new distortion, reduced central detail, or a meaningful change in vision, because posterior staphyloma is tied to macular complications that can affect prognosis. You should also be evaluated promptly if you notice a new dark bulge on the surface of the eye—especially with a history of injury—since anterior scleral staphyloma has been described after blunt trauma and may involve structural defects seen on UBM.
If you already know you have a staphyloma, follow-up timing is individualized, but the overall goal is consistent: monitor eye structure and retinal health closely enough to catch complications early and discuss options before problems become advanced.
Frequently Asked Questions (FAQ)
A staphyloma can appear as a darker area or visible bulge because the eye wall is thinned and deeper tissue can show through. Anterior scleral staphyloma may look like a black, cyst-like mass protruding from the eye surface in some reported cases.
Not exactly: high myopia refers to a high degree of nearsightedness, while posterior staphyloma is a structural outpouching of the back wall of the eye often discussed as a defining feature of pathologic myopia. In highly myopic populations, posterior staphyloma is associated with more severe myopic maculopathy and worse visual prognosis.
It can contribute to vision problems, especially when it involves the posterior pole and is associated with myopic maculopathy affecting the macula. Risk and outcome depend on the specific macular changes present, which is why imaging-based monitoring matters.
Clinicians use a dilated exam plus imaging to assess the posterior eye contour and related macular findings. Research and specialty imaging methods include swept-source OCT-based visualization/classification and emerging tools like automated posterior scleral topography for quantification.
Treatment is individualized and may include surgical removal of the protruding weak area with reinforcement using a scleral patch graft in selected cases. For advanced acquired anterior staphyloma, staged penetrating sclerokeratoplasty approaches have been reported to provide tectonic (structural) support, but they are complex and can have significant complication risks.
A staphyloma itself is often a chronic structural finding, but new symptoms can be urgent—especially sudden vision changes in highly myopic eyes or rapid changes in an anterior bulge after injury. If the eye becomes painful, vision drops suddenly, or there is new trauma, prompt evaluation is important because management can be time-sensitive.
Some causes are not fully preventable (for example, long-term remodeling in pathologic myopia), but injury prevention and timely treatment of severe infections/inflammation may reduce the chance of eye-wall weakening in some situations. For high myopia, regular monitoring is a practical way to reduce risk from complications by detecting macular disease earlier.
Key Takeaways
Staphyloma is a localized thinning and outward bulging of the sclera or cornea, often appearing darker because deeper layers show through. Posterior staphyloma is strongly linked to pathologic myopia and is associated with higher risk of myopic maculopathy and worse visual prognosis in highly myopic eyes. Anterior staphyloma can follow trauma or other eye-wall damage and may require specialist evaluation when it affects comfort, vision (through astigmatism/shape changes), or eye integrity.
Medically reviewed / Educational disclaimer
This article is for general education and is not a substitute for diagnosis or personalized treatment from an optometrist or ophthalmologist. A staphyloma’s significance depends on location and associated findings (especially macular changes in pathologic myopia), so care decisions should be made with an eye-care professional who can examine and image your eyes.
Sources and references:
- AAO EyeWiki: “Staphyloma” https://eyewiki.org/Staphyloma
- BMC Ophthalmology (PMC): Posterior staphyloma and myopic maculopathy prognosis https://pmc.ncbi.nlm.nih.gov/articles/PMC10764733/
- TVST (ARVO): Automated posterior scleral topography and staphyloma quantification https://tvst.arvojournals.org/article.aspx?articleid=2802181
- BMC Ophthalmology: Giant anterior scleral staphyloma after blunt trauma (case report) https://pubmed.ncbi.nlm.nih.gov/37964186/
- Journal of Ophthalmology (PMC): Staged penetrating sclerokeratoplasty for advanced anterior staphyloma https://pmc.ncbi.nlm.nih.gov/articles/PMC3306092/
- Ohno Matsui K Posterior staphyloma in pathologic myopia Ophthalmology 2019
Link: https://pubmed.ncbi.nlm.nih.gov/30537538/ - Posterior staphyloma in pathologic myopia Retinal Physician review https://retinalphysician.com/issues/2017/january/posterior-staphyloma-in-pathologic-myopia
- Giant anterior scleral staphyloma caused by blunt ocular trauma BMC Ophthalmology case report https://pmc.ncbi.nlm.nih.gov/articles/PMC10647092/
- Scleromalacia and anterior staphyloma clinical atlas EyeRounds University of Iowa https://eyerounds.org/atlas/pages/scleromalacia-staphyloma-glaucoma.htm