Tooth pain causing eye pain can happen because parts of the face share sensory “wiring,” so discomfort from a tooth, jaw, or nearby sinus can be felt around the eye instead of (or in addition to) the mouth. This matters because most cases are uncomfortable but not dangerous—yet a smaller number involve eye-area infections or other problems where fast evaluation helps protect vision.
A quick way to think about it: if pain seems to “travel” between an upper tooth, cheek, and the area around one eye, referred pain or sinus pressure is often on the shortlist; if eye pain comes with vision changes or difficulty moving the eye, it deserves urgent attention.
What is Tooth-to-Eye Referred Pain?
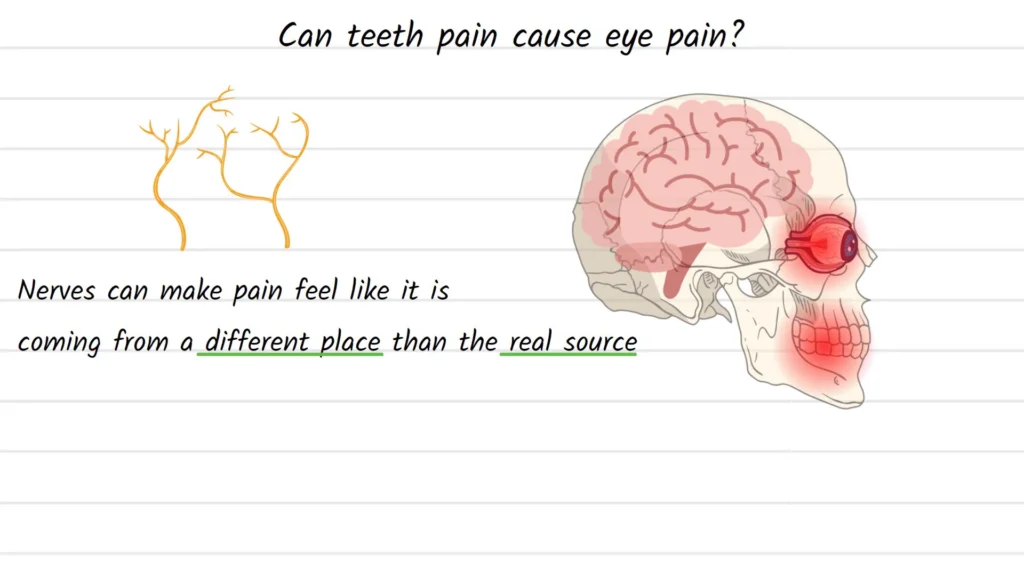
“Tooth-to-eye referred pain” isn’t a single disease—it’s a symptom pattern where pain originating in the teeth, gums, jaw, or sinuses is perceived near the eye or brow.
The main reason this happens is the trigeminal nerve (cranial nerve V), a large nerve system that carries sensation from much of the face to the brain. The trigeminal nerve has multiple branches that supply areas including the eye region and upper jaw, so the brain can sometimes misinterpret where the signal started. Cleveland Clinic describes the trigeminal nerve as a large, three-part cranial nerve that carries sensory information for wide areas of the face (and also has a chewing/motor role).
Sometimes the “pain confusion” is especially dramatic in trigeminal neuralgia, a condition that can produce intense facial pain in regions supplied by trigeminal nerve branches, including the jaw/teeth and (less often) the eye/forehead. This doesn’t mean you have trigeminal neuralgia—only that it’s a well-known example of how one nerve network can create pain in multiple facial locations.
Causes and Risk Factors
Several common situations can make tooth pain and eye-area pain show up together:
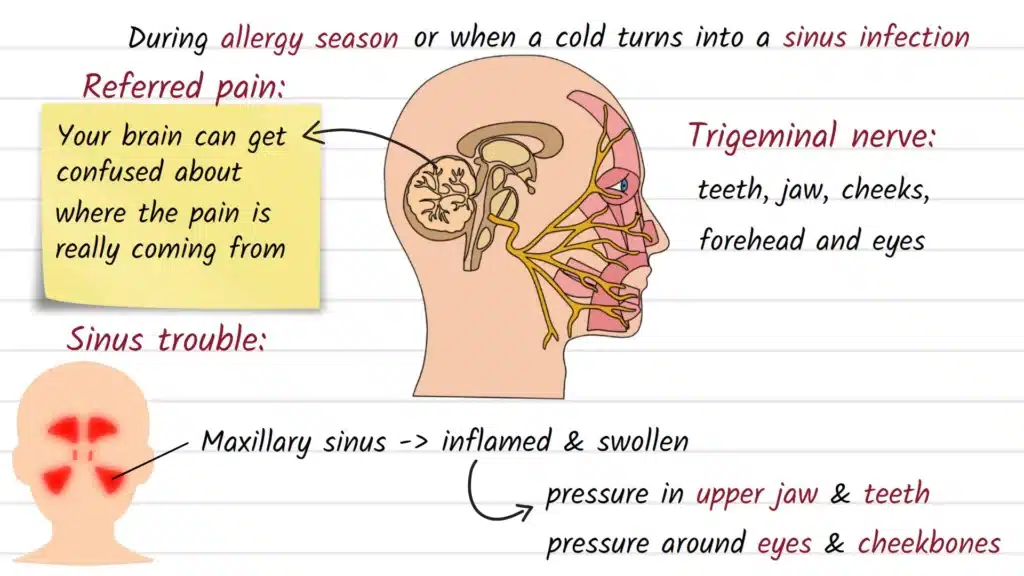
- Sinus inflammation/pressure (often maxillary sinus-related). Sinus pressure commonly feels like tightness or achiness in the face, particularly around the eyes and cheekbones, and it can radiate to the teeth and jaws.
- Sinus infection (sinusitis). Cleveland Clinic describes sinusitis as inflammation of the tissue lining the sinuses that can cause facial pain and congestion, and it’s most often triggered by viruses (like the common cold), though bacteria, fungi, and allergies can also play a role.
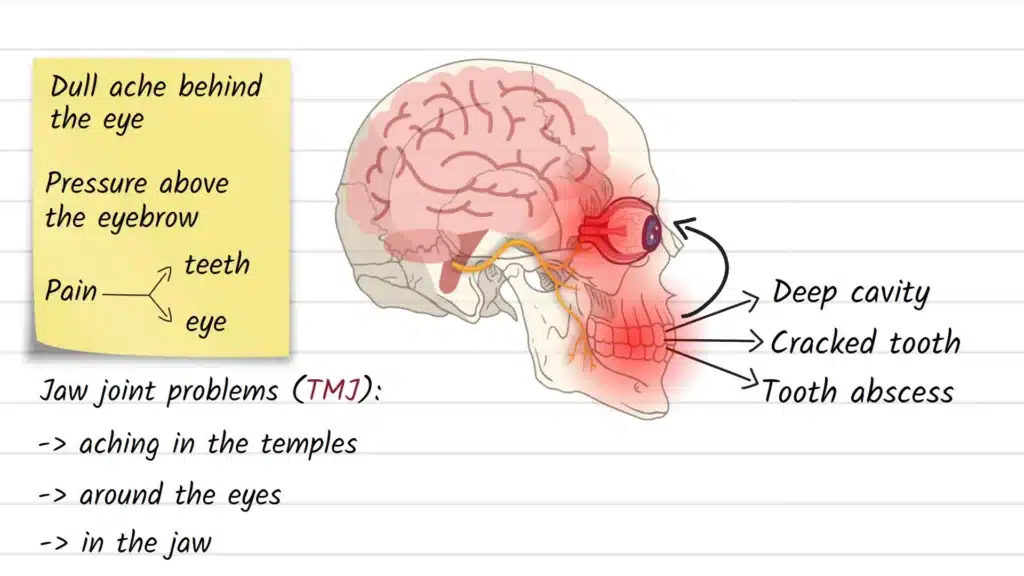
- Dental sources. Deep cavities, cracked teeth, inflamed pulp, or a dental abscess can create strong pain signals that may be felt beyond the tooth itself (for example, the cheekbone, temple, or around one eye) because those areas share facial sensory pathways (commonly discussed in the context of trigeminal nerve–mediated facial pain).
- Serious infection around/behind the eye (less common but important). Merck Manual notes that orbital cellulitis can cause eyelid and surrounding swelling/redness and may also include fever, proptosis (eye bulging), impaired ocular movement, pain with eye movements, and impaired vision.
Risk factors depend on the underlying cause. For example, viral upper-respiratory infections and allergies can contribute to sinusitis, and ongoing nasal/sinus issues can increase the chance of recurrent symptoms.
Common Signs and Symptoms
People who describe “tooth pain causing eye pain” often report one of these patterns:
- Dull ache or pressure around one eye with upper tooth discomfort on the same side.
- Heaviness or pressure across the cheeks/under the eyes, sometimes with congestion (more suggestive of sinus involvement).
- Pain that flares with chewing or biting (more suggestive of a tooth/jaw source).
If sinus pressure is part of the story, it may feel like facial tightness around the eyes, nose, forehead, or cheekbones, and it can radiate to teeth and jaws.
How the Condition is Diagnosed
Because this symptom pattern can come from teeth, sinuses, or the eye/orbit, diagnosis is usually about triage and localization—figuring out where the pain is truly originating.
A clinician may focus on:
- Timing (Did it start after a cold/allergies? Did it start after tooth sensitivity or a cracked filling?)
- Triggers (hot/cold, chewing, bending forward, nasal congestion)
- Eye-specific symptoms (vision changes, eye movement pain, swelling)
For suspected sinusitis, providers commonly diagnose it based on symptoms and history and may examine the ears, nose, and throat for swelling or drainage; Cleveland Clinic also notes that clinicians may use an endoscope to look inside the nose in some cases. If red flags suggest a deeper infection around the eye, clinicians may use imaging; Merck Manual notes that diagnosis of preseptal vs orbital cellulitis is based on history, examination, and CT or MRI.
Treatment Options Explained (non-prescriptive, informational)
Treatment depends entirely on the cause—so the “best next step” is often choosing the right professional evaluation rather than guessing.
Common pathways include:
- Dental evaluation if pain is linked to a specific tooth (especially sensitivity to temperature, pain on biting, or localized gum swelling). Dental causes may require procedures such as treating decay, addressing a crack, or draining/treating an abscess (your dentist will explain options based on findings).
- Primary care or ENT evaluation if symptoms match sinusitis (congestion, facial pressure, symptoms after a cold, pain that seems spread across the cheeks/under-eye area). Cleveland Clinic notes that sinusitis treatment options vary by duration and cause, and many cases can be managed with home care and over-the-counter measures; antibiotics may be considered when symptoms don’t improve after about 10 days or a bacterial pattern is suspected.
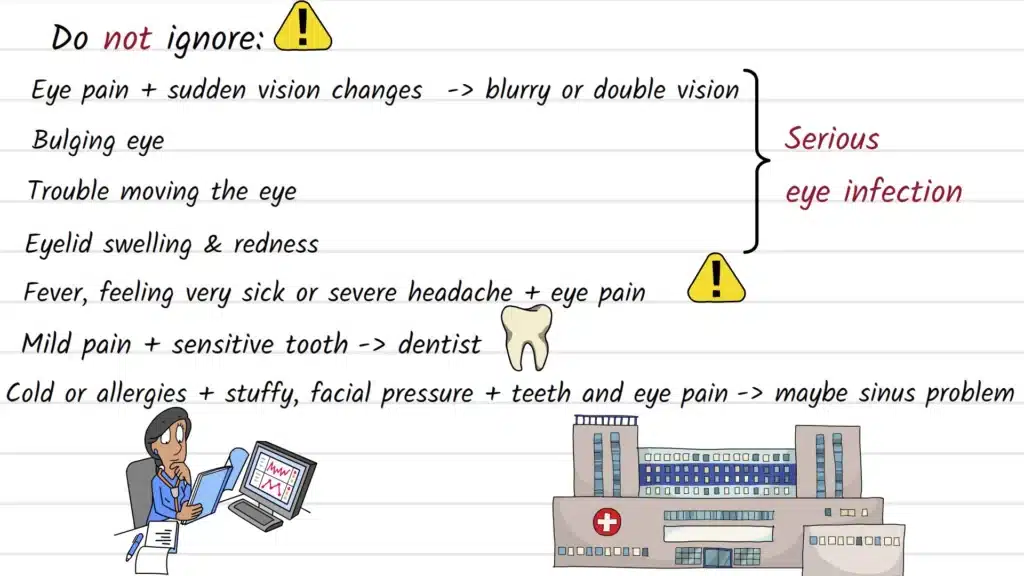
- Urgent/emergency evaluation if symptoms suggest an eye/orbital emergency. Mayo Clinic lists reasons to seek emergency care for eye pain, including sudden vision changes, swelling in or around the eyes, and trouble moving the eye, among other concerning features.
Possible Complications if Left Untreated
Most tooth-related or sinus-related pain is treatable, but complications can occur—usually when infection is involved.
- Sinusitis complications (rare). Cleveland Clinic notes that, very rarely, untreated sinus infections can lead to life-threatening infections if bacteria or fungi spread to the brain, eyes, or nearby bone.
- Orbital cellulitis complications (urgent). Merck Manual lists potential complications of orbital cellulitis including vision loss due to ischemic retinopathy/optic neuropathy from increased intraorbital pressure and intracranial spread (such as cavernous sinus thrombosis, meningitis, or brain abscess).
Because of these possibilities, worsening eye symptoms—especially with systemic illness—should be taken seriously.
Prevention and Risk Reduction (if applicable)
Prevention depends on the driver:
- If sinus infections are a recurring theme, reducing triggers (like managing allergies and avoiding respiratory infections when possible) may reduce episodes; Cleveland Clinic notes sinusitis can be triggered by viruses, bacteria, fungi, and allergens.
- If dental issues are the likely source, routine dental care and addressing tooth sensitivity early may reduce the chance of deeper tooth infections.
No prevention strategy is perfect, but earlier evaluation often prevents problems from lingering or escalating.
When to See an Eye Doctor
Consider an eye doctor (or urgent care/ER) if the pain feels like it is in the eye (not just around the eye) or if it comes with any red flags.
Mayo Clinic advises seeking emergency medical care for eye pain if it’s severe or accompanied by features such as headache/fever/light sensitivity, if vision changes suddenly, if there is swelling in or around the eyes, or if you have trouble moving the eye (among other emergency triggers). Merck Manual notes that orbital cellulitis can include pain with eye movements, decreased visual acuity, proptosis, fever, and impaired ocular movement—symptoms that warrant urgent evaluation.
If you’re unsure whether the problem is “eye vs tooth vs sinus,” it’s reasonable to start with whichever symptoms are most prominent—while prioritizing urgent evaluation for any vision change, eye movement problems, or rapidly increasing swelling.
Frequently Asked Questions (FAQ)
It can. Pain signals from the upper jaw/teeth and the eye region can share trigeminal nerve pathways, so pain may be perceived around the eye even when the source is dental.
Sinus pressure can radiate to the teeth—especially upper molars—and it often feels like tightness or achiness in the face around the eyes and cheekbones.
Sinus-related discomfort often comes with congestion and broader facial pressure around the eyes/cheeks and may follow a cold; sinusitis is inflammation of sinus-lining tissue and commonly follows viral infections. Tooth-related pain is more likely to be localized to one tooth and triggered by biting or temperature changes, though overlap is common.
Yes—especially if true eye symptoms appear. Mayo Clinic lists emergency reasons for eye pain that include sudden vision changes, swelling around the eye, and trouble moving the eye. Orbital cellulitis is one example of a serious condition that can involve pain with eye movements and decreased vision.
Merck Manual notes orbital cellulitis findings such as eyelid swelling/redness, pain with eye movements, decreased ocular motility, decreased visual acuity, proptosis, and fever. Those signs are not typical of an uncomplicated toothache and should be evaluated urgently.
Yes. Mayo Clinic describes trigeminal neuralgia as intense, shock-like pain affecting areas supplied by trigeminal nerve branches (including cheek/jaw/teeth and less often the eye/forehead). This condition has a distinct pattern and needs medical evaluation rather than self-diagnosis.
Key Takeaways
- Tooth pain causing eye pain is often explained by referred pain and shared facial sensory pathways (trigeminal nerve).
- Sinus pressure can cause pain around the eyes and can radiate to the upper teeth and jaws, which is a common reason these symptoms overlap.
- Seek urgent care for eye pain with sudden vision change, significant swelling around the eye, or trouble moving the eye; these are emergency warning signs.
Medically reviewed / Educational disclaimer
This article is for general education and does not diagnose, treat, or replace care from a dentist, optometrist, ophthalmologist, or physician. For trusted background reading, see Mayo Clinic’s guidance on when eye pain needs urgent evaluation, Merck Manual’s overview of orbital cellulitis, and Cleveland Clinic’s patient resources on sinusitis and facial/sinus pressure:
- Mayo Clinic: Eye pain—when to see a doctor — https://www.mayoclinic.org/symptoms/eye-pain/basics/when-to-see-doctor/sym-20050744
- Merck Manual: Preseptal and orbital cellulitis — https://www.merckmanuals.com/professional/eye-disorders/orbital-diseases/preseptal-and-orbital-cellulitis
- Cleveland Clinic: Sinusitis — https://my.clevelandclinic.org/health/diseases/17701-sinusitis
- Cleveland Clinic: Sinus pressure — https://my.clevelandclinic.org/health/symptoms/24690-sinus-pressure
- Mayo Clinic: Trigeminal neuralgia (symptoms/causes) — https://www.mayoclinic.org/diseases-conditions/trigeminal-neuralgia/symptoms-causes/syc-20353344
- Cleveland Clinic: Trigeminal nerve anatomy — https://my.clevelandclinic.org/health/body/21581-trigeminal-nerve