A corneal ulcer is a serious eye condition that can damage your vision very quickly if it is not treated in time. Many people first notice it as a very painful, red eye that does not improve with simple eye drops. In this guide, you will learn what a corneal ulcer is, why it happens, what symptoms to watch for, how doctors diagnose and treat it, and most importantly, how you can prevent it, especially if you wear contact lenses.
What Is a Corneal Ulcer?
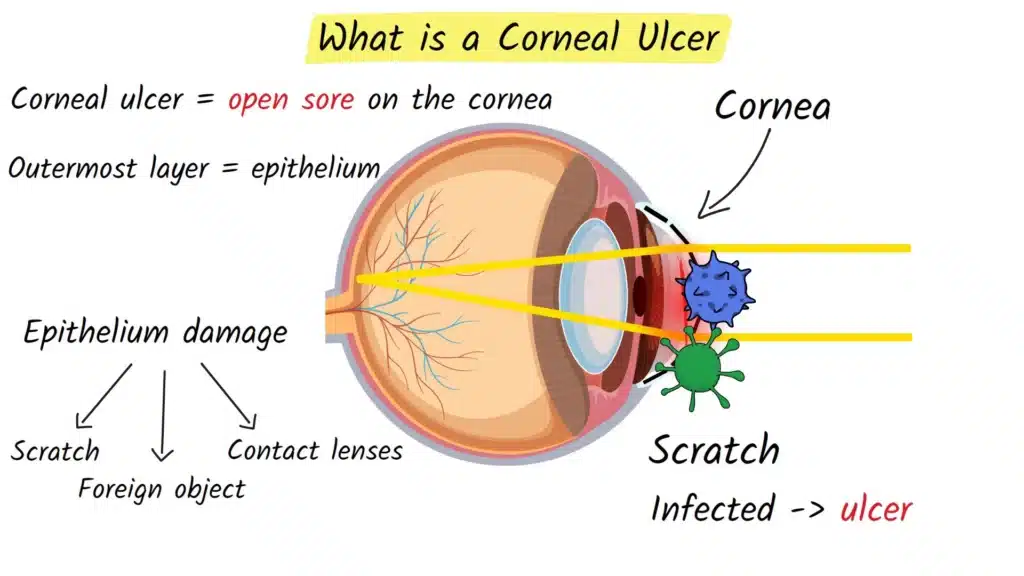
Think of your cornea as the windshield of your eye. It is the clear, dome-shaped surface at the front of the eye that covers your iris (the colored part) and your pupil (the black center). This transparent windshield protects the inside of your eye and helps focus light so you can see clearly.
Now imagine someone scratches that windshield. That scratch can become contaminated with germs and turn into an open sore or wound on the surface. That is essentially what a corneal ulcer is: an open sore on the cornea, usually caused by an infection.
The cornea itself is made up of several layers, similar to a sandwich.
- The outermost layer is called the epithelium. You can think of it as the skin of your eye.
- Beneath the epithelium are deeper layers that help maintain the cornea’s strength and clarity.
When the epithelium is damaged by a scratch, a foreign object, a chemical, or irritation from contact lenses, it creates a doorway for bacteria, viruses, or fungi to enter and infect the deeper layers. Once infection sets in, the body’s immune response and the invading organisms create that painful, inflamed sore known as a corneal ulcer.
How Does a Corneal Ulcer Develop?
A healthy cornea is normally very resistant to infection. Your tears contain natural defenses, and the epithelium acts like a smooth protective barrier. A corneal ulcer usually develops when:
- The corneal surface is broken or scratched, even by something very small, such as:
- A poorly fitting contact lens
- A speck of dust or sand
- A fingernail or makeup brush
- A tree branch or plant leaf
- Germs enter through that break. These can be:
- Bacteria
- Viruses
- Fungi
- Less commonly, parasites like Acanthamoeba (often related to contact lens use and water exposure)
- The infection grows and spreads within the cornea, causing inflammation, swelling, and tissue damage. If not treated quickly, this damage can leave a permanent scar that blocks light and reduces vision, or in extreme cases, can lead to perforation of the eye.
Corneal Ulcer Causes
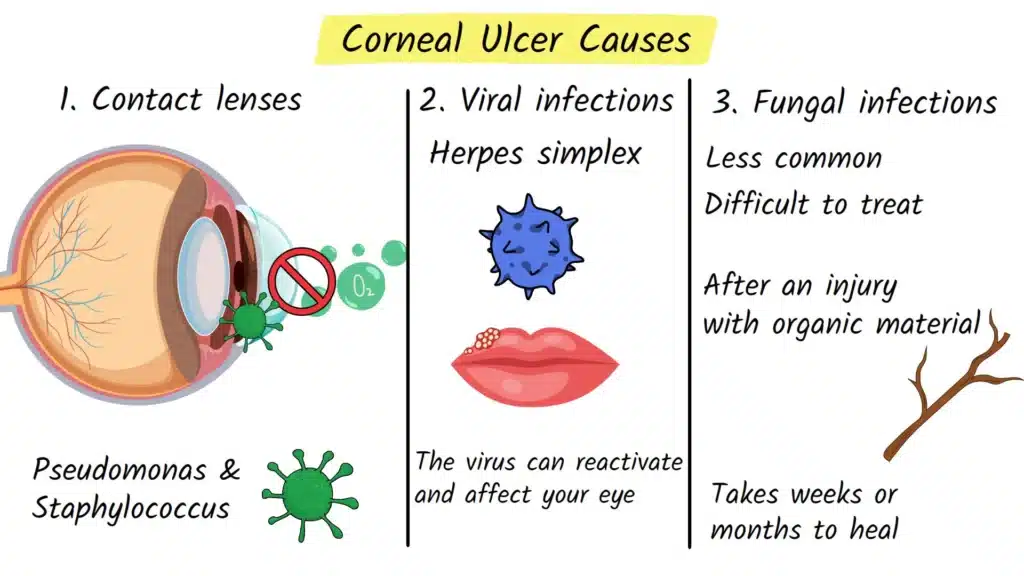
1. Contact Lenses – The Number One Risk Factor
The most common modern cause of corneal ulcers is contact lens use, especially when lenses are not worn or cleaned properly.
When you wear contact lenses, particularly if you sleep in them or wear them for long hours, you reduce the amount of oxygen reaching your cornea. This warm, moist, low-oxygen environment is perfect for bacteria to grow on the lens surface and under the lens.
If the corneal surface is slightly irritated or scratched when the lens is put in or taken out, bacteria can easily enter and cause infection. Some of the most aggressive bacteria that cause corneal ulcers include:
- Pseudomonas aeruginosa – Known for causing rapidly progressive, sight-threatening ulcers, especially in contact lens wearers.
- Staphylococcus species – Common skin bacteria that can also infect the cornea.
These infections can worsen in just a few hours, which is why any painful red eye in a contact lens wearer should be treated as urgent.
2. Viral Infections
Viral infections are another important cause of corneal ulcers. The most common virus involved is herpes simplex virus (HSV), the same virus that causes cold sores on the lips.
If you have ever had a cold sore, that virus remains in your body for life and can sometimes reactivate. When it affects the eye, it can infect the cornea and cause herpetic keratitis, a type of corneal ulcer.
Herpes-related corneal ulcers can come and go over time and may leave scars or cause thinning of the cornea. Repeated episodes can severely damage vision if not treated and monitored carefully.
3. Fungal Infections
Fungal corneal ulcers are less common than bacterial or viral ulcers, but they are often more stubborn and difficult to treat.
They usually occur after an injury with organic material, such as:
- Being poked in the eye by a tree branch, plant, or leaf
- Soil or plant debris getting into the eye
Fungi can invade the cornea and produce a slow, chronic infection that may take weeks or even months to heal. These infections are more common in hot, humid climates and in people who work outdoors, such as farmers or gardeners.
4. Other Risk Factors
Additional factors that increase the risk of corneal ulcers include:
- Dry eye disease or poor tear quality
- Eyelid problems that prevent proper blinking or eye closure
- Previous eye surgery or trauma
- Immune system problems or long-term use of steroid eye drops
Corneal Ulcer Symptoms
The symptoms of a corneal ulcer are usually intense and very difficult to ignore. People often describe the pain as severe and deep, not just a minor irritation.
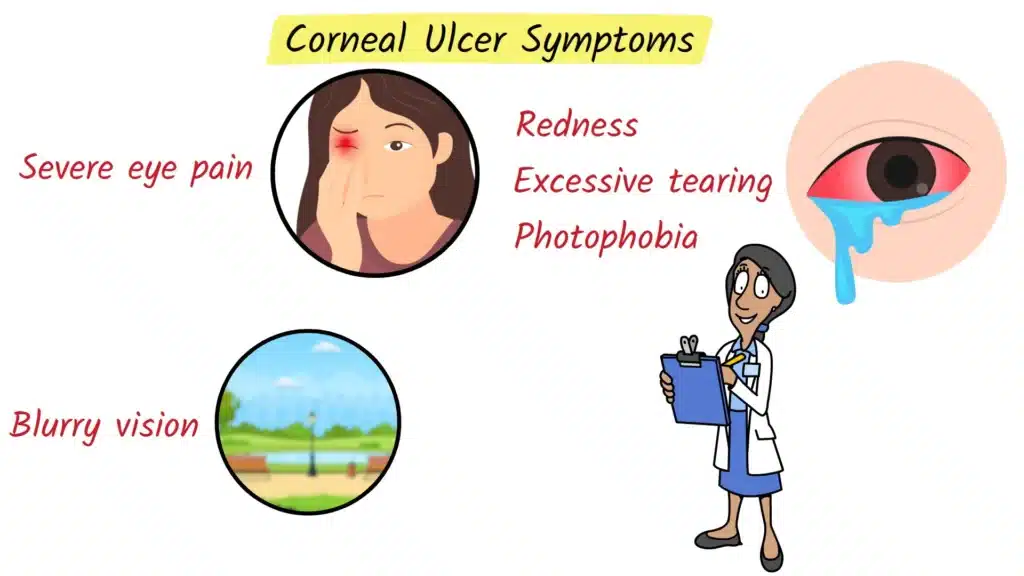
Common symptoms include:
- Severe eye pain – The kind that makes you want to keep your eye closed, because even blinking feels unbearable.
- Redness – The white part of the eye (the sclera) becomes very red and inflamed.
- Excessive tearing or discharge – The eye may water constantly or produce thick mucus or pus.
- Sensitivity to light (photophobia) – Bright light can worsen the pain and discomfort.
- Blurred or decreased vision – Your vision may become hazy, cloudy, or noticeably worse.
- A white or grayish spot on the cornea – If the ulcer is large or near the center, you may actually see a spot on the clear part of the eye when you look in the mirror.
If you wear contact lenses and notice any combination of severe pain, redness, blurred vision, or light sensitivity, remove your lenses immediately and see an eye doctor as soon as possible. Do not put the lenses back in and do not try to treat it with over-the-counter drops without professional advice.
When Is a Corneal Ulcer an Emergency?
A corneal ulcer is always serious, but it is an emergency if:
- The pain is severe and started suddenly
- Your vision drops quickly or you see a constant haze
- You notice a white spot on the cornea
- You wear contact lenses and your eye becomes very red and painful
In these situations, you should seek urgent care from an ophthalmologist or an emergency eye clinic. Early treatment can mean the difference between full recovery and permanent vision loss.
Diagnosis: How Eye Doctors Detect a Corneal Ulcer
When you visit an ophthalmologist, they will perform a detailed examination of your eye to confirm the diagnosis and identify the cause.
Typical steps include:
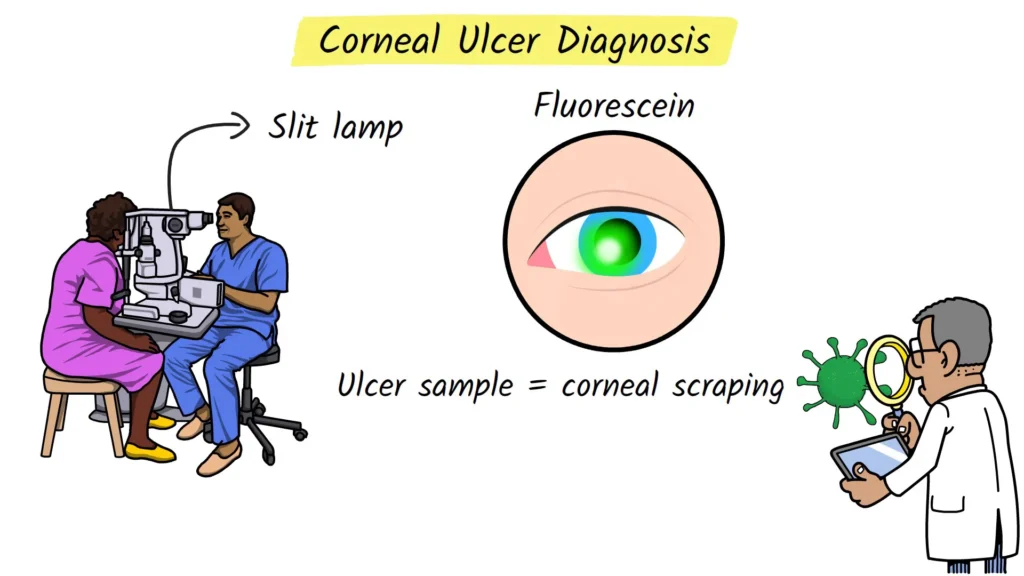
- Slit-lamp examination
The doctor uses a special microscope called a slit lamp to look at your cornea under high magnification. This allows them to see any defects, ulcers, or infiltrates (collections of inflammatory cells). - Fluorescein dye test
The doctor will place a yellow dye called fluorescein onto the surface of your eye. Under blue light, this dye makes any scratches or ulcers on the cornea glow bright green, making them much easier to see and measure. - Corneal scraping (if infection is suspected)
If an infection is likely, the ophthalmologist may gently collect a tiny sample from the ulcer using a sterile instrument. This procedure is called a corneal scraping.- The sample is sent to the lab to identify the exact organism (bacteria, fungus, or parasite).
- This helps the doctor choose the most effective, targeted medication.
Although the idea of a scraping may sound scary, it is usually done with numbing drops and takes only a few seconds. The information it provides can be extremely important in stubborn or severe cases.
Corneal Ulcer Treatment
Treatment depends on the underlying cause, but in all cases the goal is to stop the infection, reduce inflammation, control pain, and prevent scarring.
1. Bacterial Corneal Ulcers
For bacterial ulcers, your doctor will usually prescribe strong antibiotic eye drops. These may be specially compounded or high-concentration medications.
- In the beginning, you may need to use the drops every hour, even during the night, for at least the first couple of days.
- This intensive schedule is crucial, because bacterial ulcers can get much worse very quickly, especially while you sleep.
- As the infection starts to improve, your doctor will gradually reduce how often you need to use the drops.
Sometimes, if the infection is very severe or if there is a risk of deeper eye involvement, oral antibiotics or even hospital admission for around-the-clock treatment may be recommended.
2. Viral Corneal Ulcers (Herpes)
For corneal ulcers caused by herpes simplex, doctors use antiviral medications. These can be:
- Antiviral eye drops or ointments
- Oral antiviral tablets
Treatment usually continues for several days to weeks, depending on severity. In some patients who have frequent recurrences, the doctor may recommend long-term low-dose antiviral tablets to reduce the risk of future attacks.
Steroid eye drops are sometimes used later in the course of treatment to help with inflammation, but they must be prescribed and monitored very carefully by a specialist, since inappropriate steroid use can worsen some infections.
3. Fungal Corneal Ulcers
Fungal ulcers are treated with antifungal eye drops, and sometimes with oral antifungal medication as well. These infections tend to heal more slowly than bacterial ulcers.
- Treatment may be needed for weeks or even months.
- Regular follow-up is essential to monitor healing and adjust the treatment plan.
4. Surgical Options
In very severe cases, if medical treatment does not stop the infection or if the cornea becomes dangerously thin or perforated, surgery may be required.
The most common surgical treatment is a corneal transplant (penetrating keratoplasty), in which the damaged corneal tissue is removed and replaced with healthy donor tissue.
Surgery is usually considered a last resort. The main goals are to save the eye, restore the structure, and, when possible, improve vision.
Possible Complications and Long-Term Outlook
If treated early and appropriately, many corneal ulcers can heal with minimal scarring and little impact on vision. However, complications can occur, especially in severe or delayed cases:
- Permanent corneal scarring
- Astigmatism or irregular corneal shape
- Chronic dry eye or discomfort
- Thinning or perforation of the cornea
- Vision loss that may not be fully correctable with glasses or contact lenses
The prognosis depends on the size, depth, and location of the ulcer, as well as how quickly treatment is started. Ulcers in the central visual axis are more likely to affect vision long term than those at the edges of the cornea.
Corneal Ulcer Prevention
Prevention is especially important if you wear contact lenses, have had eye infections in the past, or have other risk factors.
1. Safe Contact Lens Habits
Since contact lenses are the leading cause of corneal ulcers, good lens hygiene is critical:
- Never sleep in your contact lenses unless your eye doctor has specifically told you that your lenses are approved for overnight wear and it is safe for your eyes. Sleeping in lenses raises the risk of serious infection dramatically.
- Always clean your lenses with proper contact lens solution, not with tap water, saliva, or homemade mixtures. Tap water can contain organisms like Acanthamoeba that can cause devastating corneal infections.
- Rub and rinse your lenses as directed by your eye care provider, even if the solution is labeled “no rub”.
- Replace your lens case every three months, or sooner if it becomes dirty or damaged. Clean and air-dry the case daily.
- Do not swim, shower, or use a hot tub while wearing your lenses. Water exposure while wearing lenses is a major risk factor for eye infections. If you must swim with lenses, wear waterproof goggles and remove and disinfect the lenses immediately afterward.
- Follow the replacement schedule for your lens type. Do not stretch monthly lenses to three months or daily lenses to multiple days.
If your eye becomes red, painful, or sensitive to light, remove your lenses immediately and do not put them back in until you have seen an eye doctor.
2. Protecting Your Eyes from Injury
If you do not wear contact lenses, the main way to prevent corneal ulcers is to reduce the risk of eye injuries and infections:
- Wear safety glasses or protective goggles when working with tools, cutting wood, mowing the lawn, or doing yard work.
- Use eye protection during sports and activities where objects can hit or scratch the eye.
- Avoid rubbing your eyes with dirty hands. Wash your hands frequently, especially if you have colds, skin infections, or cold sores.
3. Herpes and Other Medical Conditions
If you have a history of cold sores or known herpes infection:
- Be aware that the virus can affect your eye.
- Avoid touching a cold sore, then touching your eye.
- Discuss with your doctor whether preventive antiviral treatment is appropriate if you have had previous eye involvement.
For people with dry eye, eyelid problems, or other eye diseases, regular checkups with an eye care professional can help identify early changes before an ulcer develops.
Key Takeaways
- A corneal ulcer is an open sore on the clear front surface of the eye, usually caused by infection.
- The most common cause is contact lens misuse, especially sleeping in lenses or poor cleaning habits.
- Symptoms include severe eye pain, redness, tearing, light sensitivity, blurred vision, and sometimes a visible white spot on the cornea.
- Corneal ulcers are an eye emergency, particularly in contact lens wearers, and require rapid attention from an ophthalmologist.
- Treatment typically involves frequent antimicrobial eye drops (antibiotic, antiviral, or antifungal), and in severe cases, surgery such as a corneal transplant.
- Proper contact lens hygiene, eye protection, and hand washing are the most effective ways to prevent this serious condition.
Yes, a corneal ulcer is considered an eye emergency. Any sudden, severe eye pain, redness, light sensitivity, or blurred vision, especially in someone who wears contact lenses, should be examined by an eye doctor as soon as possible. Untreated ulcers can progress quickly, leading to permanent scarring of the cornea, vision loss, or even perforation of the eye. Early treatment greatly improves the chances of full recovery and reduces the risk of long‑term damage.
A corneal ulcer can cause permanent vision loss if it is large, deep, located in the center of the cornea, or if treatment is delayed. When the infection heals, it often leaves a scar. If that scar is in the central visual axis, it can block or distort light entering the eye, leading to blurred or reduced vision that may not be fully correctable with glasses or contact lenses. Fast diagnosis and proper treatment significantly lower the chance of serious, lasting damage.
Healing time depends on the cause, severity, and how quickly treatment is started. Mild bacterial corneal ulcers may start to improve within a few days, but usually need at least one to two weeks of treatment. Viral ulcers and especially fungal ulcers can take several weeks or even months to fully heal. Even after the infection is controlled, the cornea may continue to remodel and smooth out over time, so vision can keep improving slowly for weeks.
In many cases, people can return to contact lens wear after a corneal ulcer has completely healed, but this must be done under the guidance of an eye care professional. The doctor will check for residual scarring, corneal thinning, or dry eye that might make lens wear risky or uncomfortable. When contact lenses are reintroduced, strict hygiene is essential: no sleeping in lenses unless specifically allowed, proper cleaning with recommended solutions, avoiding water exposure, and following the replacement schedule. In some situations with severe scarring or recurrent infections, the doctor may advise against future contact lens use.
The best prevention is a combination of good hygiene and safe wearing habits. Always wash and dry your hands before handling your lenses. Never sleep in your lenses unless your eye doctor has clearly said it is safe for your specific lens type and eyes. Clean and store your lenses only in approved contact lens solution, never in tap water or saliva. Replace your lens case every three months and let it air dry between uses. Avoid swimming, showering, or using a hot tub while wearing contact lenses, because water exposure greatly increases infection risk. At the first sign of redness, pain, or blurred vision, remove your lenses and get your eyes checked promptly.
Sources
- American Academy of Ophthalmology. (2024). Corneal Ulcer: Symptoms, Causes, and Treatment.
https://eyewiki.aao.org/Corneal_Ulcer - National Eye Institute. (2023). Corneal Conditions.
https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/corneal-conditions - Kenia, H., & Sridhar, M. (2020). Microbial Keratitis: Update for General Ophthalmologists.
https://www.youtube.com/watch?v=IuI4FfwKWV8 - Red Eye MD. (2025). Corneal Ulcers: 5 Mistakes That Can WORSEN Vision Fast.
https://www.youtube.com/watch?v=Pr8MAI49_wg